The window of tolerance is the optimal zone of nervous system arousal—coined by Dan Siegel (1999)—where you can think clearly, feel emotions without overwhelm, and respond flexibly rather than react. A 2023 systematic review of 37 studies with over 2,000 participants found that attachment style measurably shapes nervous system regulation patterns (Ballesio et al., 2023), meaning your early relationships literally built the width of your window.
If you have ever gone from "fine" to "completely flooded" in seconds during a relationship conflict—or shut down and gone numb when your partner brought up something emotional—you have experienced leaving your window of tolerance. Understanding this concept through an attachment lens reveals why your nervous system responds the way it does, and what you can do about it.
Key takeaway: The window of tolerance is the arousal zone where you can think clearly and manage emotions without shutting down or spiraling. Your attachment style directly shapes how wide or narrow this window is. Anxious attachment biases toward hyperarousal, avoidant attachment creates phantom regulation that looks calm but is not, and disorganized attachment produces the most unstable window. Targeted, attachment-specific practices can widen it over time.
What Exactly Is the Window of Tolerance?
You have probably noticed your capacity for handling stress is not constant—some moments you can hold difficulty, other moments the same trigger overwhelms you. The window of tolerance is the framework that explains why. It describes three zones of nervous system arousal that determine how you respond to stress, emotion, and connection. Within the window, your prefrontal cortex stays online—you can think, feel, and choose your response. Above it, you enter hyperarousal: panic, anger, hypervigilance, racing thoughts, and the urge to fight or flee. Below it, you drop into hypoarousal: numbness, dissociation, shutdown, brain fog, and an inability to act.
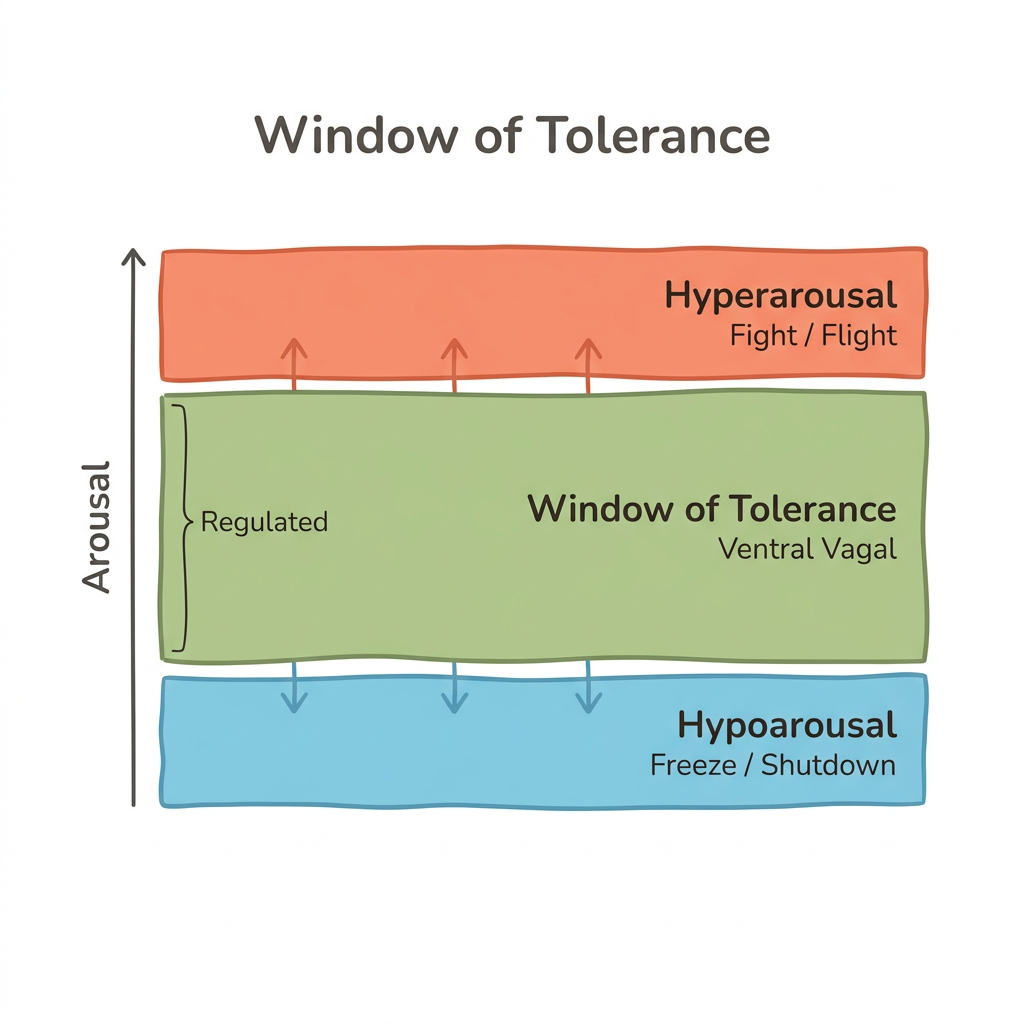
Siegel (1999) introduced this framework to describe how the autonomic nervous system moves between regulated and dysregulated states. Porges (2011) mapped these zones onto the polyvagal framework: ventral vagal activation keeps you within the window and supports social engagement. Sympathetic activation drives hyperarousal. Dorsal vagal activation drives hypoarousal—the freeze or collapse response.
What makes this model so useful is its simplicity. You do not need to analyze every emotion. You just need to know which zone you are in. Corrigan, Fisher, and Nutt (2011) confirmed that the window of tolerance model accurately describes how the autonomic nervous system responds to complex emotional trauma, with the two dysregulated zones representing distinct neurobiological states rather than just metaphors.
Your nervous system's relationship with your attachment style determines how easily you move between these zones—and how quickly you can return to the window once you have left it.
Three-Zone Body Check-In (for all attachment styles)
- Pause and notice your breathing—is it fast, slow, or held?
- Scan for muscle tension (clenched jaw, tight shoulders) versus numbness (heavy limbs, foggy head)
- Check whether you can think clearly or if your thoughts are racing or blank
- Label your zone out loud: "I'm in my window," "I'm above it," or "I'm below it"
This builds interoceptive awareness—the ability to read your own body's signals. Interoception is the foundation of widening the window because you cannot regulate what you cannot detect. For anxious attachment, it interrupts the spiral before it peaks. For avoidant attachment, it catches the shutdown your mind might dismiss as "being fine."
How Does Your Attachment Style Shape Your Window?
Your attachment style determines the default width and bias of your window of tolerance. Mikulincer and Shaver (2003, 2007) identified two core nervous system strategies—hyperactivation and deactivation—that map directly onto how each attachment style experiences arousal regulation.
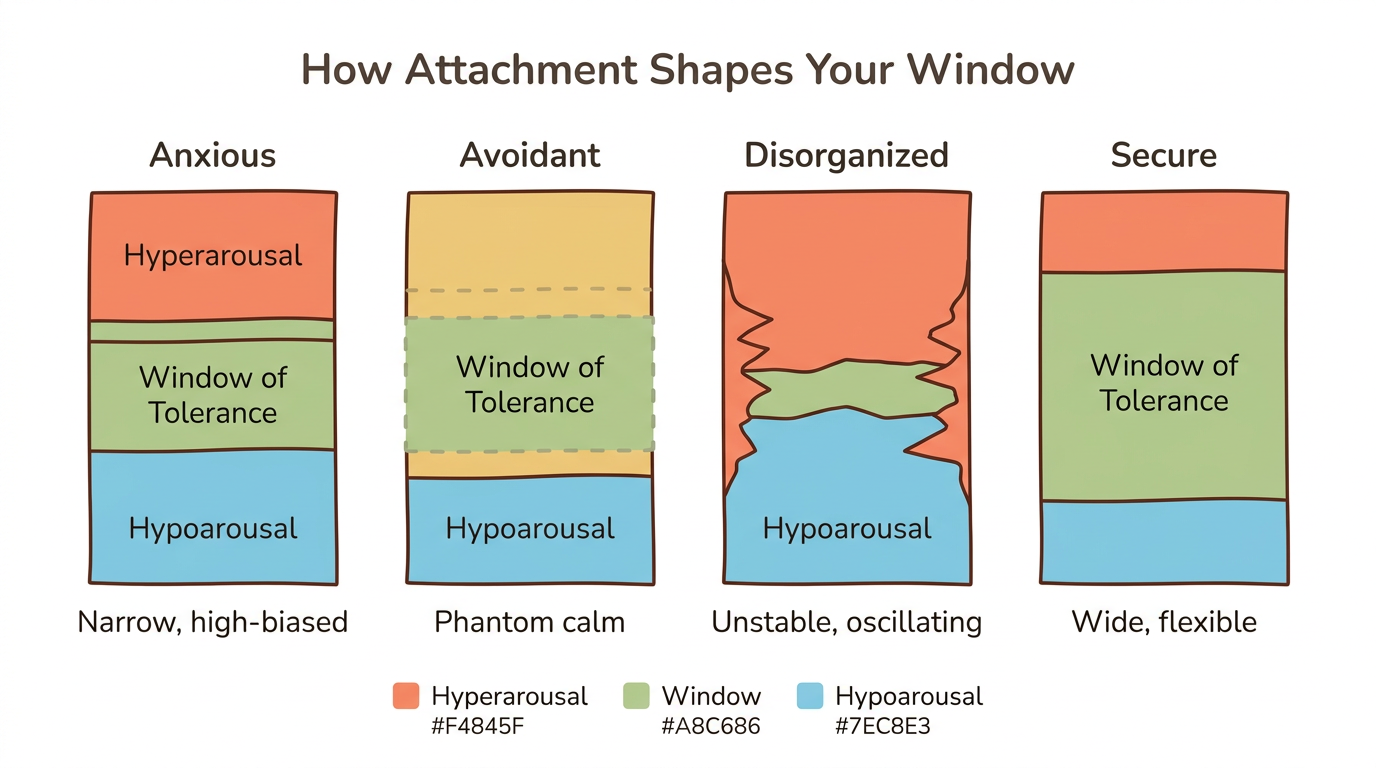
Anxious and Preoccupied Attachment
Picture this: your partner takes two hours to reply to a text, and by the time they respond, your heart is pounding and you have drafted three follow-up messages. That escalation is not overreaction—it is your nervous system leaving its regulated zone. Hyperactivating strategies chronically intensify emotions and heighten threat monitoring (Mikulincer and Shaver, 2003), and your window is narrow and biased toward the upper edge. Your nervous system learned to amplify distress signals because that was the strategy most likely to get a response from an inconsistent caregiver. A partner's delayed text or a shift in tone can push you above your window within seconds—that familiar panic is your nervous system doing exactly what it was trained to do.
Dismissive-Avoidant Attachment
You genuinely believe you are calm. Your face is relaxed, your voice is steady, and if someone asked how you feel, you would say "fine" and mean it. But Ballesio et al. (2023) documented what is happening underneath: "phantom regulation." Dismissing individuals report feeling fine but show elevated sympathetic activation and skin conductance. The deactivation strategy works at the conscious level, but the body stays stressed. Your window appears wide, but physiologically it is narrow. The same review found that dismissing mothers showed anterior insula activation—a brain region associated with disgust—when hearing infant distress cries. The suppression is real, and it costs your body something.
Disorganized and Fearful-Avoidant Attachment
Instability defines the disorganized window. Rather than consistently going up or down, your nervous system oscillates unpredictably between hyperarousal and hypoarousal—sometimes within the same conversation. Ballesio et al. (2023) found elevated amygdala activation and impaired prefrontal regulation in unresolved individuals—the brain's alarm system fires loudly while the rational brain struggles to come online. Fearful-avoidant patterns reflect this oscillation: wanting closeness triggers fear, which triggers withdrawal, which triggers longing, in a cycle that never settles.
Secure Attachment
A wide and flexible window characterizes secure attachment. Ballesio et al. (2023) documented adaptive heart rate variability patterns—decreasing during stress and recovering quickly afterward—along with higher oxytocin responses and lower cortisol. Secure individuals can move toward the edges of their window without falling out. Strong emotions arise, and the nervous system returns to baseline without getting stuck.
| Attachment Style | Window Width | Dominant Zone | Nervous System Strategy | What It Feels Like | Key Expansion Strategy | Physiological Marker |
|---|---|---|---|---|---|---|
| Anxious | Narrow, high-biased | Hyperarousal | Hyperactivating | Racing thoughts, need for reassurance, panic | Downregulation and grounding | Elevated cortisol, rapid HRV increase |
| Dismissive-Avoidant | Apparently wide, physiologically narrow | Hypoarousal (conscious); Hyperarousal (physiological) | Deactivating ("phantom regulation") | "I'm fine" while body holds tension | Upregulation and feeling-access | Elevated skin conductance despite behavioral calm |
| Disorganized | Narrowest and unstable | Both—oscillating | No consistent strategy | Unpredictable swings between flooding and numbness | Pendulation and safety anchoring | Elevated amygdala, impaired PFC, erratic HRV |
| Secure | Wide and flexible | Rarely dysregulated; recovers quickly | Flexible, adaptive | Can feel strong emotions and return to baseline | Continued co-regulation and resilience | Adaptive HRV, higher oxytocin, lower cortisol |
Window Mapping Journal (for all attachment styles)
- Track three moments this week when you felt emotionally activated in a relationship
- Note whether you went up (racing heart, urgency, heat) or down (numbness, fog, heaviness)
- Identify the trigger—was it an attachment cue like silence, conflict, vulnerability, or closeness?
- Add your attachment-specific layer: Anxious? Notice if you moved up first. Avoidant? Check your body signals even when you feel "fine." Disorganized? Notice if you swung between both zones
- After a week, look for your pattern—this is your window signature
This exercise works because it makes your automatic pattern visible. Anxious attachment hyperactivates so quickly that the spiral feels like reality rather than a nervous system response. Avoidant attachment deactivates below conscious awareness—journaling catches what your mind filters out. Disorganized attachment oscillates so fast that slowing down to track each shift builds the predictability your nervous system never learned.
What Happens in Your Brain When You Leave the Window?
When you leave your window of tolerance, your prefrontal cortex goes offline and your amygdala takes over—meaning you lose access to rational thought and enter survival mode. Research using fMRI and PET imaging shows a significant inverse correlation between medial prefrontal cortex activity and amygdala activity (Shin et al., 2005). This amygdala-PFC seesaw explains why you cannot think your way out of a triggered state—the part of your brain responsible for rational thought has literally powered down.
Within the window, your prefrontal cortex regulates the amygdala like a skilled supervisor managing an alarm system. It evaluates whether the threat is real, modulates the intensity of the response, and chooses an appropriate action. When activation pushes you outside the window, the amygdala overwhelms prefrontal control. Your alarm system starts running the show, and every ambiguous signal reads as danger.
For avoidant attachment, this seesaw operates with a twist. Ballesio et al. (2023) found that dismissing individuals show elevated sympathetic nervous system activity despite behavioral calm—meaning the amygdala is activated, but the conscious experience has been disconnected from the body's stress signals. The PFC goes offline in a different way: instead of being flooded, it is overriding body signals at a cost.
Oxytocin functions as a natural window-expander. Secure attachment is associated with higher baseline oxytocin, and research has shown that intranasal oxytocin decreases amygdala reactivity in insecurely attached individuals (Riem et al., cited in Ballesio et al., 2023). Secure mothers show greater oxytocin and lower cortisol responses to their infants. HRV serves as a measurable marker of window width—secure attachment correlates with adaptive HRV that drops during stress and recovers afterward, while disorganized attachment shows elevated HRV throughout recovery, revealing the effortful suppression happening beneath the surface (Ballesio et al., 2023).
Vagal Tone Reset (somatic and body-based—targets all styles, especially anxious activation)
- Breathe with an extended exhale: inhale through your nose for 4 counts, exhale slowly through your mouth for 6 to 8 counts. Continue for 2 minutes
- On three of those exhales, hum or sing a low note—this vibrates the vagus nerve where it passes through the throat
- Place one hand on your chest and one on your belly, noticing if your breathing shifts from shallow chest breathing to deeper belly breathing
- Name one thing you can see, one thing you can hear, and one thing you can physically feel right now
This activates the ventral vagal system—the social engagement pathway that Porges (2011) identified as the neurobiological foundation of feeling safe. The extended exhale directly stimulates the vagus nerve, shifting your autonomic state from sympathetic fight-or-flight toward ventral vagal regulation. For anxious attachment, this counteracts the sympathetic hijack that drives protest behavior. The humming adds vagal toning that generic deep breathing misses.
Why Does Childhood Attachment Narrow the Window?
Secure caregiving builds a wide window through consistent co-regulation, while insecure caregiving narrows the window by teaching the nervous system that distress is unmanageable. When a caregiver consistently responds to a child's distress with attuned presence—soothing, containing, and co-regulating—the child's nervous system learns a foundational lesson: activation is temporary, and I can return to baseline. That learning becomes the width of the window.
When caregiving is inconsistent, absent, or frightening, the lesson changes. The child's nervous system learns that distress may not end, that reaching for comfort may be ignored or punished, and that the only reliable regulation is whatever the child can generate alone. Pat Ogden described the "dyadic dance" of secure attachment as the original window-widening mechanism (Ogden, Minton, and Pain, 2006)—the synchronized rhythm between caregiver and child that teaches the nervous system how to move through activation and return to calm.
Corrigan, Fisher, and Nutt (2011) documented how childhood abuse narrows the window so severely that dysfunctional behaviors—self-harm, substance use, disordered eating—become attempts to regulate an overwhelmed nervous system that readily tips into extreme states. These are not character flaws. They are a nervous system reaching for the only regulation tools available when the window has been compressed to almost nothing.
Approximately 40 to 45 percent of adults in Western populations have insecure attachment styles (Mickelson, Kessler, and Shaver, 1997). That means nearly half of adults are operating with a narrower window than they could have—not because something is wrong with them, but because their nervous systems adapted to the relational environments they grew up in.
Safe Anchor Visualization (somatic—especially for disorganized attachment)
- Recall a moment—even a brief one—when you felt genuinely safe with another person. This could be a friend's laugh, a pet's warmth, or a therapist's steady voice
- Notice where in your body you feel that safety: warmth in your chest, softness in your belly, settling in your shoulders
- Breathe into that body sensation for 60 seconds, letting it spread slightly with each exhale
- Assign it a word or image—"warm," "held," "golden"—as an anchor you can return to
For disorganized attachment, safety itself can feel threatening because the original source of safety was also the source of danger. This exercise builds a somatic reference point for what "within the window" actually feels like in the body. It works with implicit body memory rather than cognitive override—you are not trying to convince yourself you are safe, you are giving your nervous system a felt experience to reference.
How Can You Expand Your Window of Tolerance?
Your nervous system learned its current pattern for good reason. It kept you regulated in the environment you had. And now you can gradually teach it something new—not through force, but through repeated small experiences of safety.
You can expand your window of tolerance through attachment-style-specific practices, safe relationships, and targeted therapy. The key insight most generic advice misses: the strategies that widen an anxious person's window are different from those that widen an avoidant person's window. Your nervous system needs the specific intervention it did not receive—not a one-size-fits-all approach.
1. For Anxious Attachment—Downregulation Practices
Your window narrows upward, biased toward hyperarousal. Grounding techniques, extended exhale breathing, bilateral stimulation like alternating taps, and containment imagery all help bring your nervous system down from that activated state. You are not managing crises—you are learning to self-soothe so thoroughly that your baseline drops. You are teaching your body that the absence of intensity is not the same as the absence of connection.
2. For Avoidant Attachment—Upregulation and Feeling-Access
Beneath the phantom calm, your body is holding tension, grief, and need that the deactivating strategy has pushed underground. Body scanning for suppressed sensations, graduated emotional exposure, and naming emotions with specificity all help surface what is actually happening. What this builds is not overwhelm—it is the capacity to notice what your body already knows beneath the composed exterior.
3. For Disorganized Attachment—Pendulation and Safety Anchoring
Instability defines the disorganized window, so predictability is what your nervous system needs most. Titrated oscillation between activation and settling—what Somatic Experiencing calls pendulation—teaches the nervous system that it can move between states without getting stuck. Never force full immersion into distress. Small, contained doses of activation followed by deliberate settling build the nervous system's confidence that it can regulate.
4. For All Styles—Co-regulation
Co-regulation is not weakness—it is neurobiology. Safe relationships literally widen your window. Porges (2011) identified the social engagement system as the ventral vagal pathway—eye contact, warm vocal tone, physical proximity with safe people all activate this system. Emotionally Focused Therapy research demonstrates that restructuring attachment bonds in couples directly expands each partner's window. When you communicate your needs to a responsive partner, you are not just resolving a conflict—you are widening your window through lived relational experience.
5. For All Styles—Targeted Therapy Modalities
Sensorimotor Psychotherapy (Ogden et al., 2006) works directly within the window of tolerance framework using body-based interventions for attachment and developmental trauma. EMDR uses the window of tolerance as a preparatory phase, expanding it before processing traumatic material. Emotionally Focused Therapy restructures attachment bonds through co-regulation. Internal Family Systems identifies protective parts that push you into hyper or hypoarousal. Therapy can change your attachment style—and the window of tolerance is one of the primary mechanisms through which that change happens.
Pendulation Practice (somatic—especially for disorganized and fearful-avoidant attachment)
- Notice an area of tension or discomfort in your body—maybe a tight chest, clenched stomach, or aching shoulders
- Now notice an area of ease or neutrality—perhaps your hands, your feet, or the back of your neck
- Gently shift your attention to the area of discomfort. Stay with it for 20 to 30 seconds, just noticing
- Shift to the area of ease. Stay for 20 to 30 seconds, letting your attention rest there
- Repeat 3 to 4 times, noticing if the discomfort softens even slightly
- End by resting your attention on the area of ease for a full minute
This teaches the nervous system that activation is not permanent and that it can return to regulation—directly counteracting the disorganized pattern of getting stuck in extreme states. Unlike grounding exercises that only pull you down from hyperarousal, pendulation works with both zones by showing your body it can move between them voluntarily. That voluntary movement is what your nervous system never learned from unpredictable caregiving.
Can Your Window of Tolerance Change Permanently?
Yes—neuroplasticity research confirms that the window of tolerance can widen permanently through repeated experiences of safe regulation. The brain rewires attachment-related neural pathways throughout adulthood, and measurable changes in HRV, cortisol patterns, and amygdala reactivity have been documented across treatment studies (Ballesio et al., 2023). The window you have now is not the window you are stuck with.
This widening process parallels what attachment researchers call earned security—the shift from insecure to secure attachment patterns through therapy, reflective awareness, and reparative relationships (Mikulincer and Shaver, 2024). Developing secure attachment as an adult is not about erasing your history. It is about giving your nervous system enough new experiences that its default range expands.
You do not rewire your window in a single insight. You rewire it by noticing 10 percent earlier that you have left your window, responding 10 percent differently, 10 percent more often. Over months, those small shifts accumulate into a nervous system that can hold more without collapsing or exploding.
The window of tolerance is not a fixed trait—it is a living, responsive system that reflects your cumulative relational experiences. Every time you notice activation without acting on it, every time a safe person co-regulates with you, every time you practice returning to your body instead of fleeing from it, the window widens slightly. Neuroplasticity means these changes are structural, not just behavioral. Your brain is literally building new neural pathways each time you practice.
Window Width Timeline (reflective—for all attachment styles)
- Think back to a situation one to two years ago that would have overwhelmed you—a conflict, a silence, a vulnerability
- Notice honestly how you would respond to it today. Has anything shifted?
- Identify what changed: a relationship, a practice, therapy, self-awareness, or simply time with safer people
- Write down one concrete thing that widened your window
This builds awareness that your window has already been changing, countering the hopelessness that often accompanies insecure attachment. Recognizing past growth is not toxic positivity—it is evidence your nervous system collects to justify taking the next small risk. When your body has proof it has expanded before, the next expansion feels less impossible.
When Should You Seek Professional Support?
Seeking professional help is itself a co-regulation strategy—it is using the attachment system as designed. Your nervous system was built to regulate in relationship with others, and a therapist provides the consistent, attuned presence that may have been missing from early caregiving.
Some signs that self-guided practices are not enough:
- Frequent dissociation or losing time
- Inability to return to your window without substances, self-harm, or other harmful behaviors
- Trauma flashbacks or intrusive memories that hijack your nervous system
- Relationship patterns that consistently re-narrow your window despite genuine effort
- Feeling unsafe in your own body most of the time
Corrigan, Fisher, and Nutt (2011) documented that dysfunctional regulation behaviors often represent a nervous system that has been pushed beyond what individual strategies can manage. Approximately 70 percent of people experience significant trauma, and those with narrower windows are more vulnerable to developing lasting effects.
Specific therapy modalities that work explicitly with the window of tolerance include Sensorimotor Psychotherapy, EMDR, Somatic Experiencing, Emotionally Focused Therapy, and Internal Family Systems. Each approaches the window from a different angle—body, bilateral processing, relationship, or parts work—and the right therapy can shift your attachment style over time. Using the attachment system as designed means reaching for safe connection when your own resources are not enough. That is not failure. That is the system working.
Frequently Asked Questions
What is the window of tolerance?
The window of tolerance is the optimal zone of nervous system arousal—coined by Dan Siegel in 1999—where you can think clearly, feel emotions without overwhelm, and respond flexibly. Above the window is hyperarousal, marked by panic and anger. Below the window is hypoarousal, marked by numbness and shutdown.
How do I know if I'm outside my window of tolerance?
Hyperarousal signs include racing heart, rapid thoughts, anger, anxiety, and an urge to fight or flee. Hypoarousal signs include emotional numbness, brain fog, feeling disconnected from your body, fatigue, and an inability to think clearly or take action.
What causes a narrow window of tolerance?
Inconsistent, absent, or frightening caregiving in childhood narrows the window by training the nervous system to stay on high alert. Trauma, chronic stress, and insecure attachment all contribute. Ballesio et al. (2023) found that disorganized attachment produces the narrowest effective window of tolerance.
Is the window of tolerance the same as emotional regulation?
The window of tolerance describes your nervous system's capacity range, while emotional regulation refers to the strategies you use to stay within or return to that range. Think of the window as the container and emotional regulation as the skills you use to stay inside it.
Can your window of tolerance change?
Yes. Neuroplasticity research confirms the window can widen through therapy, safe relationships, somatic practices, and consistent co-regulation. Measurable changes in heart rate variability, cortisol, and amygdala reactivity have been documented across treatment studies. The window you have now is not permanent.
How does childhood trauma affect the window of tolerance?
Childhood trauma narrows the window by conditioning the autonomic nervous system to react to smaller triggers with larger stress responses. Corrigan, Fisher, and Nutt (2011) found that behaviors like self-harm and substance use often represent attempts to regulate a nervous system that readily tips into extreme states.
What is the window of tolerance in polyvagal theory?
In polyvagal terms, the window of tolerance maps to ventral vagal activation—the social engagement system where you feel safe enough to connect. Hyperarousal corresponds to sympathetic fight-or-flight activation, and hypoarousal corresponds to dorsal vagal freeze or shutdown responses.
What are the best exercises to expand the window of tolerance?
Effective exercises include extended-exhale breathing, vagal toning through humming, pendulation between body sensations, grounding techniques, and co-regulation with safe people. The most effective approach targets your specific attachment style rather than relying on generic techniques.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Foundational Works
- Siegel, D. J. (1999). The Developing Mind: Toward a Neurobiology of Interpersonal Experience. Guilford Press.
- Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation. Norton.
- Ogden, P., Minton, K., & Pain, C. (2006). Trauma and the Body: A Sensorimotor Approach to Psychotherapy. Norton.
Attachment and Emotion Regulation
- Mikulincer, M., & Shaver, P. R. (2003). Attachment theory and affect regulation: The dynamics, development, and cognitive consequences of attachment-related strategies. Motivation and Emotion, 27(2), 77–102.
- Mikulincer, M., & Shaver, P. R. (2024). Attachment orientations and emotion regulation: New insights from integrative reviews. Current Opinion in Psychology. PMC10849076.
- Ballesio, A., et al. (2023). Attachment-related differences in emotion regulation in adults: A systematic review of neurophysiological and psychobiological studies. Brain Sciences, 13(6), 884.
- Mickelson, K. D., Kessler, R. C., & Shaver, P. R. (1997). Adult attachment in a nationally representative sample. Journal of Personality and Social Psychology, 73(5), 1092–1106.
Neuroscience and Trauma
- Corrigan, F. M., Fisher, J. J., & Nutt, D. J. (2011). Autonomic dysregulation and the Window of Tolerance model of the effects of complex emotional trauma. Journal of Psychopharmacology, 25(1), 17–25.
- Shin, L. M., et al. (2005). A functional magnetic resonance imaging study of amygdala and medial prefrontal cortex responses to overtly presented fearful faces in posttraumatic stress disorder. Archives of General Psychiatry, 62(3), 273–281.
This article is for educational purposes only and is not a substitute for professional mental health treatment. If you are experiencing significant distress, dissociation, or trauma symptoms, please consult a licensed mental health professional who specializes in attachment and trauma.
