Disorganized attachment is a pattern where a person simultaneously desires and fears intimacy, rooted in early experiences where the caregiver was both the source of safety and the source of threat. A landmark meta-analysis of over 6,000 infant-parent dyads found that approximately 15 percent of the general population develops disorganized attachment, rising to 25 to 80 percent in clinical and maltreatment populations (van IJzendoorn, Schuengel, and Bakermans-Kranenburg, 1999).
If you have ever felt like you are the one pulling someone close and pushing them away in the same breath — or if your partner does this to you — something deeper than mixed signals is at work. Your nervous system learned a paradox early in life: the person you needed most was also the person who frightened you. This article will walk you through the neuroscience, the felt experience, and the concrete path toward healing.
Key takeaway: Disorganized attachment, also called fearful-avoidant attachment, develops when a caregiver is both the source of comfort and fear. Affecting approximately 15 percent of the general population, it creates a push-pull pattern of simultaneously craving and fearing closeness. Research spanning over two decades shows that healing to earned secure attachment is achievable through therapy, somatic work, and corrective relational experiences.
What Exactly Is Disorganized Attachment?
Disorganized attachment is what researchers call a "collapse in behavioral and attentional strategies" — it is not a strategy at all, but the absence of one (Hesse and Main, 2000). Unlike anxious attachment, which organizes around pursuit, or avoidant attachment, which organizes around withdrawal, disorganized attachment means your system never settled on a coherent way to cope with relational distress.
Main and Hesse (1990, 2006) coined the term "fright without solution" to describe how this pattern forms. Imagine being a small child. You are frightened — maybe by a loud noise, a bad dream, or the caregiver themselves. Every mammalian instinct drives you toward your caregiver for safety. But what happens when the caregiver is the source of the fear? You cannot approach (danger) and you cannot flee (you depend on them for survival). The system crashes.
This is not a character flaw. It is the most logical response to an impossible situation.
Disorganized attachment affects approximately 15 percent of the general population in normative samples (van IJzendoorn et al., 1999). In populations with histories of maltreatment, that number rises dramatically — between 25 and 80 percent. If you recognize this pattern in yourself, you are far from alone.
The Push-Pull Inventory
- Reflect on 3 recent relationship moments where you felt conflicted about closeness
- For each moment, write down: What closeness did I crave? What did I fear about that closeness? What did I actually do?
- Look across all three — notice any pattern of oscillating between moving toward and pulling away
- Name the pattern without judging it: "I notice I tend to _____ when I feel _____"
- Sit with that awareness for 30 seconds, placing a hand over your heart
Is Disorganized Attachment the Same as Fearful-Avoidant?
Yes — disorganized and fearful-avoidant describe the same core pattern, measured in different developmental contexts. "Disorganized" comes from Mary Main and Judith Solomon's infant research using the Strange Situation procedure, while "fearful-avoidant" comes from Bartholomew and Horowitz's (1991) adult four-category model published in the Journal of Personality and Social Psychology.
The distinction matters because it explains why you might encounter both terms and feel confused. In Bartholomew's model, fearful-avoidant attachment is defined by a negative self-image AND negative image of others — "I am not worthy of love, and others cannot be trusted to provide it." This dual negativity is what makes it distinct from anxious attachment (negative self, positive other) or avoidant attachment (positive self, negative other).
Here are the four adult attachment categories in Bartholomew's model:
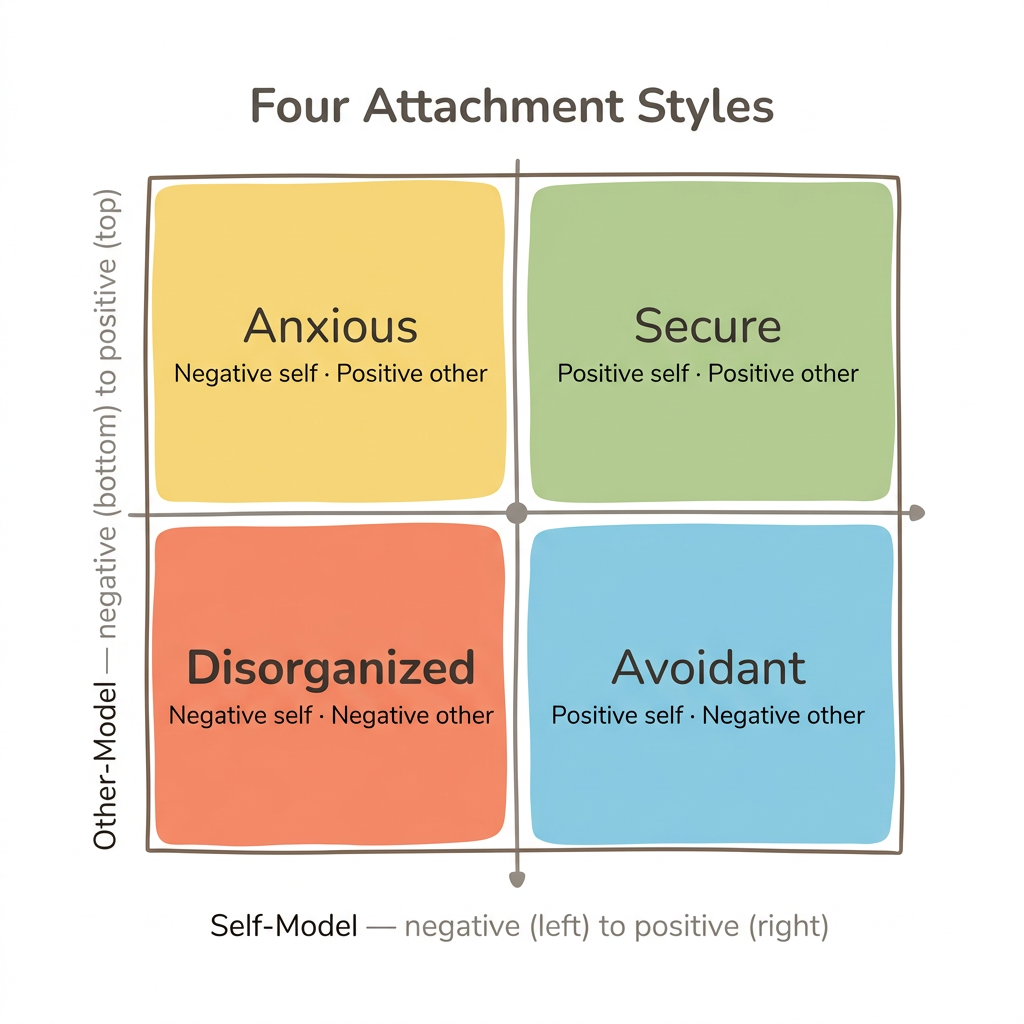
- Secure — Positive self-model, positive other-model: "I am worthy of love, and others are generally trustworthy"
- Preoccupied (anxious) — Negative self-model, positive other-model: "I am not enough, but if I try hard enough, others can save me"
- Dismissive (avoidant) — Positive self-model, negative other-model: "I am fine on my own, and others are unreliable"
- Fearful (disorganized) — Negative self-model, negative other-model: "I am not worthy, and others are dangerous"
When you see either term in research or self-help content, know they point to the same lived experience: the painful oscillation between needing closeness and fearing it.
What Causes Disorganized Attachment in Childhood and Adulthood?
Disorganized attachment develops through three primary pathways, all rooted in the same paradox — the caregiver being both source of safety and source of fear. A meta-analysis by Madigan et al. (2006) of 851 infant-parent dyads found that infants whose parents displayed frightened or frightening behavior were 3.7 times more likely to develop disorganized attachment.
Frightened or Frightening Caregiving
The parent who rages and then comforts. The caregiver who dissociates during feeding or bathing, becoming emotionally absent while physically present. The parent whose face suddenly goes blank or fearful for reasons the child cannot understand. These behaviors do not need to be constant — intermittent unpredictability is enough to prevent the child's nervous system from settling on a coherent strategy.
Overt Maltreatment
Children who experience abuse or neglect face 4 times the odds of developing disorganized attachment. In maltreatment populations, prevalence rises to 25 to 80 percent (van IJzendoorn et al., 1999). The child's protector is their threat — the definition of fright without solution.
Unresolved Parental Trauma
This is the pathway that surprises most people. A parent does not need to be abusive to transmit disorganization. A parent carrying their own unresolved grief, loss, or trauma may subtly dissociate during caregiving, display moments of inexplicable fear, or oscillate between emotional availability and emotional absence. Research suggests a 70 percent intergenerational transmission rate of attachment insecurity — meaning the wounds travel forward, often without anyone recognizing it.
Your nervous system learned this pattern for a good reason. It kept you safe in an environment where no single strategy could work. That is not something to be ashamed of. It is something to understand.
Mapping Your Caregiving Landscape
- Draw two columns on a piece of paper: "Safe Moments" and "Frightening or Confusing Moments"
- Think about your primary caregiver — write specific memories in each column
- Notice if the same person appears in both columns
- Notice any feelings arising as you see this on paper — tightness, numbness, sadness
- Place a hand on your belly and take 3 slow breaths. Remind yourself: "This is about understanding, not blaming"
What Are the Signs of Disorganized Attachment in Adults?
The signs of disorganized attachment in adults cluster into three recognizable patterns: an anxious side, an avoidant side, and a disorganized core where both activate simultaneously. The systematic review by Pollard et al. (2023) in the British Journal of Clinical Psychology confirmed that self-report measures of disorganized attachment consistently correlate with depression, anxiety, and trauma symptoms.
The Anxious Side
Hypervigilance to partner's mood shifts. Reading abandonment into minor changes — a delayed text, a shift in tone. Protest behaviors: calling repeatedly, seeking reassurance, struggling to self-soothe. If this resonates, you may also recognize the signs of anxious attachment in yourself.
The Avoidant Side
Emotional shutdown when things get too close. Deactivating strategies: suddenly feeling "nothing" after intense connection. Pushing partners away after moments of vulnerability. Convincing yourself you do not need anyone. These deactivating strategies overlap with avoidant attachment patterns, but in disorganized attachment, they alternate with the anxious behaviors rather than being consistent.
The Disorganized Core
Rapid oscillation between the two sides — sometimes within the same conversation. Dissociation during conflict — going blank, feeling foggy, or losing track of what you were arguing about. Testing and sabotaging relationships to see if the other person will stay. Difficulty constructing a coherent narrative about your own life and relationships.
One striking finding from a study published in Nature Scientific Reports (2020): people with disorganized attachment perceive gentle touch as unpleasant, while securely attached individuals rate the same caress-like touch as pleasant. Your body learned that closeness — even tender closeness — might mean danger.
Window of Tolerance Check-In (body-based practice)
- Set 3 reminders on your phone throughout one day
- At each reminder, place a hand on your chest and pause for 15 seconds
- Notice: Am I in fight or flight (heart racing, tension, urge to flee or argue)? Freeze (numb, foggy, heavy, collapsed)? Or my window of tolerance (calm but alert)?
- Name the state silently without judgment: "I notice activation" or "I notice shutdown"
- Track your states over one week to identify your baseline patterns
How Does Disorganized Attachment Show Up in Romantic Relationships?
Disorganized attachment creates a recurring relationship cycle that often feels inescapable: idealization, rising anxiety, testing, conflict escalation, emotional shutdown, rupture, desperate repair, and then back to idealization. Research suggests that fearful-avoidant couples experience significantly higher conflict escalation rates compared to other attachment pairings (Mikulincer & Shaver, 2016).
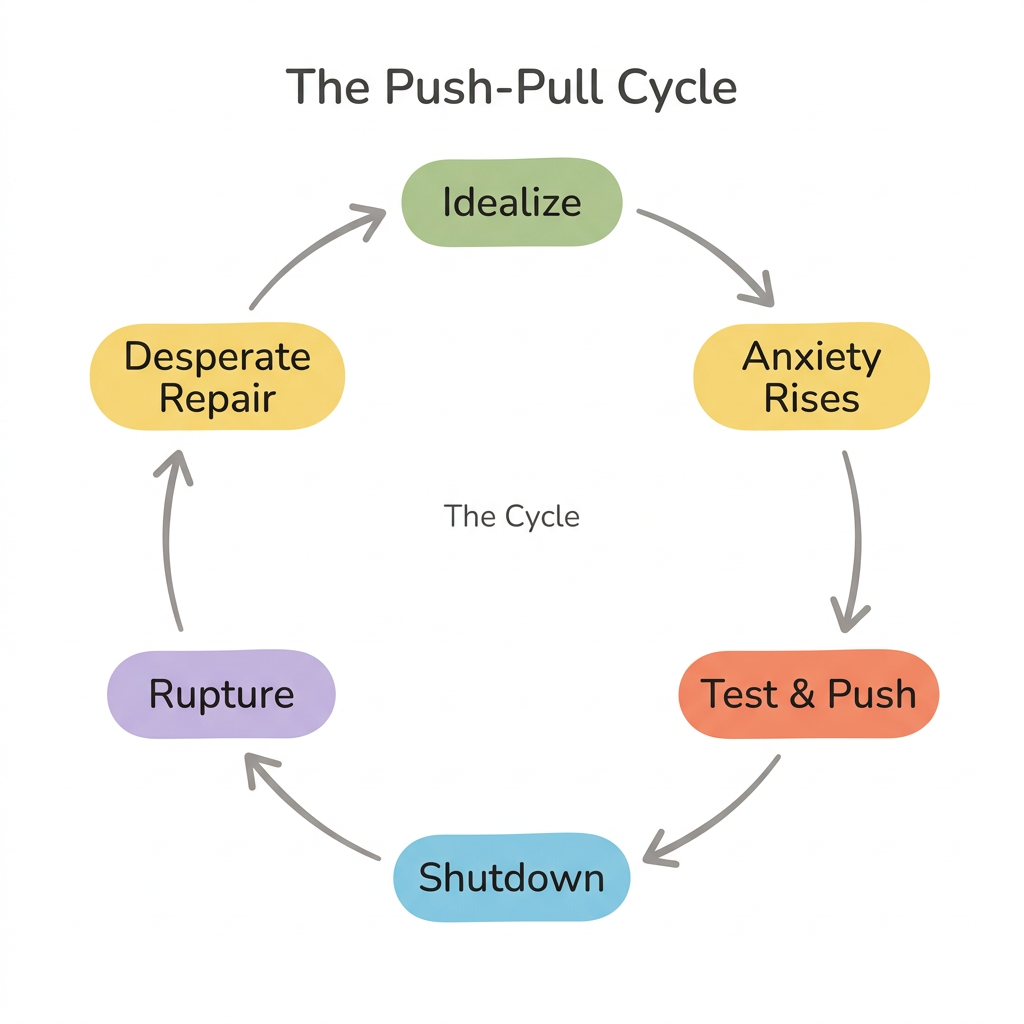
The Cycle From the Inside
You meet someone and feel a powerful pull. Early connection feels electric — maybe even like "this person finally gets me." Then closeness triggers your threat response. You begin testing: picking fights, withdrawing affection, creating distance to see if they will stay. When they pull back in response, abandonment fear floods in and you pursue desperately. This is fright without solution in adult form — your nervous system replaying the original paradox.
Specific patterns include difficulty with sexual vulnerability, trouble accepting kindness without suspicion, and preemptive abandonment — leaving before the other person can leave you. Research also links disorganized attachment to chronic loneliness: 42 percent of adults who report chronic loneliness have disorganized attachment (YouGov survey data).
The Partner's Perspective
Partners often describe feeling like they are on a rollercoaster — unsure whether to give space or move closer. The common advice to "just be consistent" is correct in principle but insufficient in practice. Consistency helps, but understanding the nervous system dynamics underneath the behavior is what transforms a relationship from surviving to healing.
That texting panic your partner experiences when you do not respond immediately? That is their attachment system activating — the anxious side of the disorganized pattern firing hard.
Relationship Cycle Mapping
- Draw a circle on paper and mark these phases around it: Honeymoon, Anxiety Rising, Testing or Pushing, Withdrawal, Crisis, Desperate Reconnection
- Identify where you tend to get stuck — which phase lasts longest for you?
- Note what body sensations accompany each phase (chest tightness, stomach dropping, numbness)
- Identify one phase where you could insert a 30-second pause before reacting
- Write one sentence you could say to yourself at that pause point: "I notice I'm in the _____ phase"
Disorganized Versus Anxious Versus Avoidant Attachment: Key Differences
| Dimension | Anxious (Preoccupied) | Avoidant (Dismissive) | Disorganized (Fearful-Avoidant) |
|---|---|---|---|
| Core fear | Abandonment | Engulfment or loss of independence | Both abandonment AND engulfment |
| Self-model | Negative ("I'm not enough") | Positive ("I don't need anyone") | Negative ("I'm not worthy") |
| Other-model | Positive ("They can save me") | Negative ("Others are unreliable") | Negative ("Others are dangerous") |
| Strategy | Hyperactivation (pursue) | Deactivation (withdraw) | No coherent strategy (oscillate) |
| In conflict | Pursue, protest, seek reassurance | Stonewall, withdraw, minimize | Oscillate between pursuing and withdrawing |
| Nervous system | Sympathetic dominant (fight or flight) | Dorsal vagal dominant (shutdown) | Blended states (fight or flight and freeze simultaneously) |
| Prevalence | Approximately 20 percent of adults | Approximately 25 percent of adults | Approximately 15 to 20 percent of adults |
What Happens in Your Nervous System With Disorganized Attachment?
Disorganized attachment creates a state where your nervous system fires simultaneous fight/flight AND freeze responses — your body cannot decide whether to run toward safety or collapse, so it does both at once. This is why you can feel panicked and numb at the same time.
The Polyvagal Lens
Stephen Porges's polyvagal theory describes three autonomic states: ventral vagal (safe and social), sympathetic (fight or flight), and dorsal vagal (freeze and collapse). Most people with insecure attachment lean toward one: anxious attachment tends toward sympathetic activation, avoidant attachment tends toward dorsal vagal shutdown. Disorganized attachment is unique because it involves blended autonomic states — both systems firing simultaneously without resolution.
This is the somatic signature of fright without solution. Your nervous system learned that closeness equals danger, but aloneness also equals danger. There is no safe resting state.
What the Brain Research Shows
Prospective studies spanning 18 to 22 years found that disorganized attachment in infancy predicts greater amygdala volume in adulthood — your brain's threat detection center literally grows larger (PMC, 2023). Neuroimaging research also reveals altered resting-state connectivity: higher connectivity between the right amygdala and anterior cingulate cortex (hypervigilant threat monitoring) and lower connectivity between the left amygdala and cerebellum (impaired motor regulation) (PubMed, 2021).
Additionally, infants with disorganized attachment show a flattened diurnal cortisol rhythm (n = 369) — meaning their stress hormone system has lost its natural rise-and-fall pattern. The system is chronically activated, eventually becoming "burned out" and unable to mount appropriate stress responses. This is not a personal failing. This is your biology adapting to an environment where threat was unpredictable.
Autonomic State Body Scan (somatic practice)
- Find a quiet seated position and close your eyes if comfortable
- Starting from your feet, slowly scan upward through your body
- Notice areas of tension, heat, or restlessness — these suggest sympathetic activation
- Notice areas of numbness, heaviness, or cold — these suggest dorsal vagal shutdown
- Place a hand on any area where you notice both sensations existing close together
- Breathe into that area for 5 slow breaths
- Whisper to yourself: "I notice this. I am safe right now." This begins the process of differentiating blended states
Can Disorganized Attachment Be Healed?
Yes — and the evidence is strong. Longitudinal research spanning 23 years demonstrates that people with disorganized attachment histories can develop what researchers call "earned secure attachment" — secure adult functioning built through therapy, corrective relational experiences, and the development of a coherent self-narrative about one's past.
Healing disorganized attachment is not erasing the past but integrating it. Earned-secure individuals can talk about painful childhood experiences with clarity, compassion, and coherence — without becoming flooded or dismissive. Their nervous systems develop the flexibility to move between autonomic states rather than getting stuck in blended activation.
Several evidence-based modalities show particular promise:
- Internal Family Systems (IFS) — Works with the internal fragmentation characteristic of disorganized attachment, helping you develop Self-leadership to hold opposing impulses without being overwhelmed by either
- Somatic Experiencing — Directly addresses the freeze and collapse responses stored in the body, reprogramming your nervous system's threat response to closeness
- EMDR (Eye Movement Desensitization and Reprocessing) — Targets unresolved trauma memories that fuel the fright-without-solution pattern, helping reprocess frightening caregiver experiences
- Emotionally Focused Therapy (EFT) — The most empirically validated couples therapy, with over 90 percent of couples reporting significant improvements. EFT helps both partners see and break the pursue-withdraw cycle
- DBT (Dialectical Behavior Therapy) — Distress tolerance and emotion regulation skills address the emotional dysregulation central to disorganized attachment. The dialectic of acceptance AND change mirrors the both-and nature of the disorganized experience
One Rung of the Ladder
- Name one relationship pattern you want to change — be specific (for example, "I shut down during arguments")
- Identify the smallest possible experiment — not a transformation, just one rung (for example, "Stay in the room 30 seconds longer during a disagreement instead of leaving")
- Try it once this week
- Afterward, notice what your nervous system does — without requiring it to feel comfortable
- Write down what you observed. That observation IS the progress
You do not rewire attachment in a single insight. You rewire it by noticing 10 percent earlier, responding 10 percent differently, 10 percent more often.
How Can You Support a Partner With Disorganized Attachment?
Supporting a partner with disorganized attachment requires consistency without pressure — being reliably present without demanding vulnerability on your timeline. Your partner's nervous system is watching for evidence that closeness is dangerous. Every moment you remain calm and available, you provide counter-evidence.
Here are practical strategies grounded in polyvagal co-regulation principles:
- Name the pattern, not the person — Say "I notice we are in the push-pull cycle right now" instead of "You are pushing me away again." This externalizes the pattern and reduces shame
- Regulate your own nervous system first — You cannot co-regulate from a dysregulated state. Your calm nervous system is the most powerful intervention available
- Tolerate the oscillation without personalizing it — When your partner withdraws after closeness, it is not about you. Their nervous system is responding to closeness as threat. This is reflexive, not intentional
- Set boundaries with compassion — Attachment style is an explanation, not an excuse. You can understand the pattern without accepting harmful behavior. "I understand you are activated, and I am not willing to be yelled at" is a complete sentence
- Consider couples therapy — EFT provides a structured container where both partners can learn to identify and interrupt the cycle with professional support
The Co-Regulation Pause
- When you sense the push-pull activating, take 3 slow breaths before responding
- Say: "I am here. I am not going anywhere. And I do not need anything from you right now"
- Allow silence — resist the urge to fill it
- If your partner withdraws, remain calm and available without pursuing
- If they escalate, name the cycle: "I think we are both activated right now. Can we take 10 minutes and come back to this?"
When Should You Seek Professional Help for Disorganized Attachment?
Seek professional support when disorganized attachment patterns are interfering with your daily functioning or causing repeated relational harm. Disorganized attachment specifically benefits from relational healing — a corrective attachment experience with a therapist who provides the consistent, non-threatening presence your nervous system needs to rewire.
Consider professional help when:
- Dissociation is frequent — you regularly go blank, feel foggy, or lose time during emotional conversations
- Relationships consistently end in the same destructive cycle — you can see the pattern but cannot stop it alone
- Emotional flashbacks occur during intimacy — moments where present closeness triggers past fear
- You notice controlling or harmful behaviors emerging in yourself or accepting them from partners
- Depression, anxiety, or trauma symptoms are persistent — research confirms strong associations between disorganized attachment and clinical conditions, including a 60 percent association with borderline personality traits and a 55 percent association with dissociative symptoms (Pollard et al., 2023)
Some researchers, including Lyons-Ruth and colleagues, frame borderline personality disorder as a "generalization of disorganized attachment." Having disorganized attachment does not mean you have BPD — they are distinct constructs. But if you are experiencing emotional intensity that feels beyond your capacity to manage, a therapist trained in attachment and trauma can help you distinguish what is happening and build a path forward.
Look for therapists trained in IFS, Somatic Experiencing, EMDR, or EFT. Ask specifically about their experience with attachment-based work and trauma. The therapeutic relationship itself becomes a laboratory for new relational patterns — a place where your nervous system can practice trust in small, safe doses.
Frequently Asked Questions
Is disorganized attachment the same as fearful-avoidant?
Yes, disorganized and fearful-avoidant describe the same core pattern. "Disorganized" comes from infant research by Main and Solomon (1990) using the Strange Situation procedure, while "fearful-avoidant" comes from Bartholomew and Horowitz's 1991 adult attachment model. Both describe simultaneously craving and fearing closeness due to a caregiver who was both source of comfort and source of fear.
Is disorganized attachment the worst attachment style?
No attachment style is "the worst," but disorganized attachment is considered the most challenging because it lacks a coherent coping strategy. Research links disorganized attachment to higher rates of emotional distress, relationship conflict, and clinical conditions. However, longitudinal studies demonstrate that people can develop earned secure attachment through therapy and corrective relational experiences.
Can disorganized attachment be healed?
Yes. Research on earned secure attachment — spanning 23-year longitudinal studies — shows that people with disorganized histories can develop secure functioning. Effective approaches include IFS, EMDR, Somatic Experiencing, and Emotionally Focused Therapy. Healing does not erase the past but builds new neural pathways for experiencing safety in connection.
What causes disorganized attachment?
Disorganized attachment develops when a caregiver is simultaneously the source of comfort and fear — what researchers call fright without solution. Causes include abuse, neglect, or a parent's own unresolved trauma creating frightened or dissociative caregiving behavior. A meta-analysis by Madigan et al. (2006) found children of frightened or frightening parents are 3.7 times more likely to develop disorganized attachment.
How does disorganized attachment affect romantic relationships?
Disorganized attachment creates a push-pull dynamic: craving intimacy while fearing it. Research suggests fearful-avoidant couples experience significantly higher conflict escalation rates. The cycle typically involves idealization, testing, emotional shutdown, rupture, and desperate repair. Partners often describe feeling like they are on a rollercoaster, unsure whether to give space or pursue closeness.
What therapy is best for disorganized attachment?
Evidence-based approaches include Internal Family Systems for internal fragmentation, Somatic Experiencing for the freeze response, EMDR for reprocessing caregiver trauma, and Emotionally Focused Therapy for couples with over 90 percent reporting significant improvement. DBT also helps with emotion regulation. The most effective therapy addresses both psychological patterns and the body's stored trauma responses.
When someone with disorganized attachment pushes you away, should you give space or stay?
Both, strategically. Offer consistent, calm presence without pursuing or pressuring. Communicate something like "I am here when you are ready" and mean it. Avoid chasing, which triggers fear of engulfment, or disappearing, which triggers abandonment fear. Focus on regulating your own nervous system first — you cannot co-regulate from a dysregulated state.
Is disorganized attachment linked to BPD?
Research shows approximately 60 percent of individuals with borderline personality disorder display disorganized or fearful-avoidant attachment. Some researchers frame BPD as a generalization of disorganized attachment patterns. However, having disorganized attachment does not mean you have or will develop BPD — they are distinct but overlapping constructs with different diagnostic criteria.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Foundational Works
- Main, M., & Hesse, E. (1990). Parents' unresolved traumatic experiences are related to infant disorganized attachment status: Is frightened and/or frightening parental behavior the linking mechanism? In M. T. Greenberg, D. Cicchetti, & E. M. Cummings (Eds.), Attachment in the preschool years (pp. 161–182). University of Chicago Press.
- Hesse, E., & Main, M. (2000). Disorganized infant, child, and adult attachment: Collapse in behavioral and attentional strategies. Journal of the American Psychoanalytic Association, 48(4), 1097–1127.
- Bartholomew, K., & Horowitz, L. M. (1991). Attachment styles among young adults: A test of a four-category model. Journal of Personality and Social Psychology, 61(2), 226–244.
- Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation. W. W. Norton.
Research Studies and Meta-Analyses
- van IJzendoorn, M. H., Schuengel, C., & Bakermans-Kranenburg, M. J. (1999). Disorganized attachment in early childhood: Meta-analysis of precursors, concomitants, and sequelae. Development and Psychopathology, 11(2), 225–250. Meta-analysis, N > 6,000 infant-parent dyads.
- Madigan, S., Bakermans-Kranenburg, M. J., van IJzendoorn, M. H., Moran, G., Pederson, D. R., & Benoit, D. (2006). Unresolved states of mind, anomalous parental behavior, and disorganized attachment: A review and meta-analysis of a transmission gap. Attachment & Human Development, 8(2), 89–111. Meta-analysis, N = 851.
- Pollard, R., et al. (2023). Measures of adult disorganized attachment: A systematic review. British Journal of Clinical Psychology.
- Nature Scientific Reports (2020). Altered touch perception in disorganized attachment: Caress-like stimuli rated as unpleasant by disorganized-attachment adults.
Neuroscience and Physiology
- PMC (2023). Prospective neuroimaging studies (18–22 year span): Disorganized infant attachment predicts greater amygdala volume in adulthood.
- PubMed (2021). Resting-state fMRI: Altered amygdala-anterior cingulate cortex connectivity in adults with disorganized attachment.
- PMC (2023). Flattened diurnal cortisol rhythm in infants with disorganized attachment, n = 369.
Clinical and Applied Sources
- Lyons-Ruth, K., et al. BPD as a generalization of disorganized attachment. Frontiers in Psychology (2018); PMC.
- PMC (2016). Disorganized attachment mediates the link between childhood abuse severity and dissociative symptoms.
- PMC (2024) and Attachment Project. Earned secure attachment: Longitudinal evidence across 23-year studies.
- EFT efficacy research: Over 90% of couples report significant improvements in attachment security.
Aggregated Statistics
- WifiTalents. Attachment style statistics compilation (aggregated from multiple sources).
- YouGov. Attachment and loneliness survey data.
This article is for educational purposes only and is not a substitute for professional mental health advice, diagnosis, or treatment. If you are experiencing distress related to attachment patterns, please consult a licensed mental health professional. If you are in crisis, contact the 988 Suicide and Crisis Lifeline by calling or texting 988.
