Relationship overthinking is the repetitive, unproductive analysis of a partner's words, behaviors, or the relationship's future — distinct from healthy reflection. Approximately 73 percent of adults aged 25 to 35 report chronic overthinking (Nolen-Hoeksema, 2003), and 25 percent of all rumination is triggered by interpersonal situations.
This pattern is not a personal failing. It is a signal from your attachment system — the part of your brain wired to monitor connection and threat. Different attachment styles overthink in different ways: anxious attachment drives hypervigilance about abandonment, avoidant attachment produces post-withdrawal analysis, and fearful-avoidant attachment oscillates between both. What follows is the neuroscience behind relationship rumination, attachment-specific patterns, and evidence-based techniques to break the cycle.
Key takeaway: Relationship overthinking is driven by your attachment system, not a character flaw. Approximately 73 percent of young adults ruminate, and attachment anxiety is the strongest predictor. The antidote is not just stop thinking — it is regulating your nervous system, distinguishing attachment alarms from real threats, and building secure communication patterns with your partner.
Why Does Your Brain Get Stuck in Relationship Overthinking?
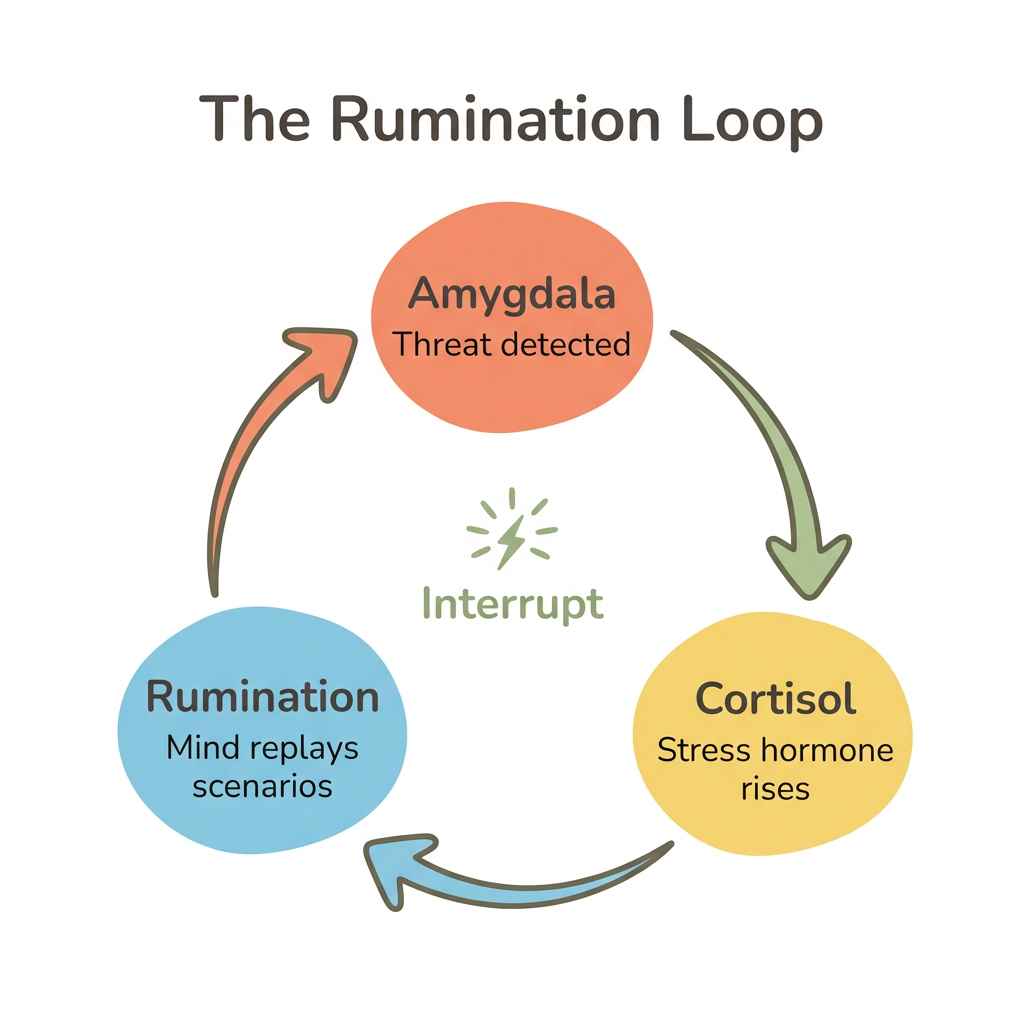
If you have ever spent an entire evening replaying a single conversation, you know how draining this cycle can be. The exhaustion is real — and it has a neurological explanation. Your brain gets stuck in relationship overthinking because of a feedback loop between three neural systems: the default mode network, the threat-detection system, and the stress hormone cortisol. When these systems lock into a cycle, your mind replays relationship scenarios on an involuntary loop.
The default mode network is your brain's "mind-wandering network" — the regions that activate when you are not focused on a task. In people who ruminate, the subgenual prefrontal cortex connects too tightly to this network, creating what researchers describe as "a functional neural ensemble well-suited for depressive rumination" (Hamilton et al., 2015). Your nervous system essentially hijacks your daydreaming circuits and fills them with worst-case relationship scenarios.
Meanwhile, the amygdala-prefrontal cortex circuit — your brain's threat-detection system — stays "stuck on" regardless of actual danger. Stronger structural connections between these regions predict lower anxiety (Kim and Whalen, 2009). In overthinkers, this circuit responds to ambiguity as if it were threat. A delayed text gets processed the same way as a genuine warning sign.
Then cortisol seals the loop. State rumination is consistently linked to increased cortisol concentrations and greater cortisol reactivity (Zoccola and Dickerson, 2012). More cortisol means heightened threat sensitivity. Heightened threat sensitivity means more rumination. The cortisol feedback loop keeps spinning until something interrupts it — and that something is rarely willpower alone.
"Name the Network" Awareness Check (for all attachment styles)
- Notice when you have been replaying a relationship scenario
- Say internally: "My default mode network just activated. This is my brain's autopilot, not reality."
- Name one thing you can see right now
- Name one thing you can hear
- Name one thing you can physically feel (feet on floor, air on skin)
This cognitive defusion technique externalizes the mental process, weakening your identification with the thoughts. By naming the brain network responsible, you create distance between you and the rumination — you are observing the pattern rather than being consumed by it.
How Does Your Attachment Style Shape Your Overthinking?
Your attachment style determines what you overthink about, when the rumination peaks, and how it shows up in your behavior. Research shows that rumination fully mediates the link between anxious attachment and psychological distress (Burnette et al., 2009) — meaning overthinking is not a side effect of insecure attachment but the primary mechanism through which it causes suffering.
Here are the four distinct overthinking patterns:
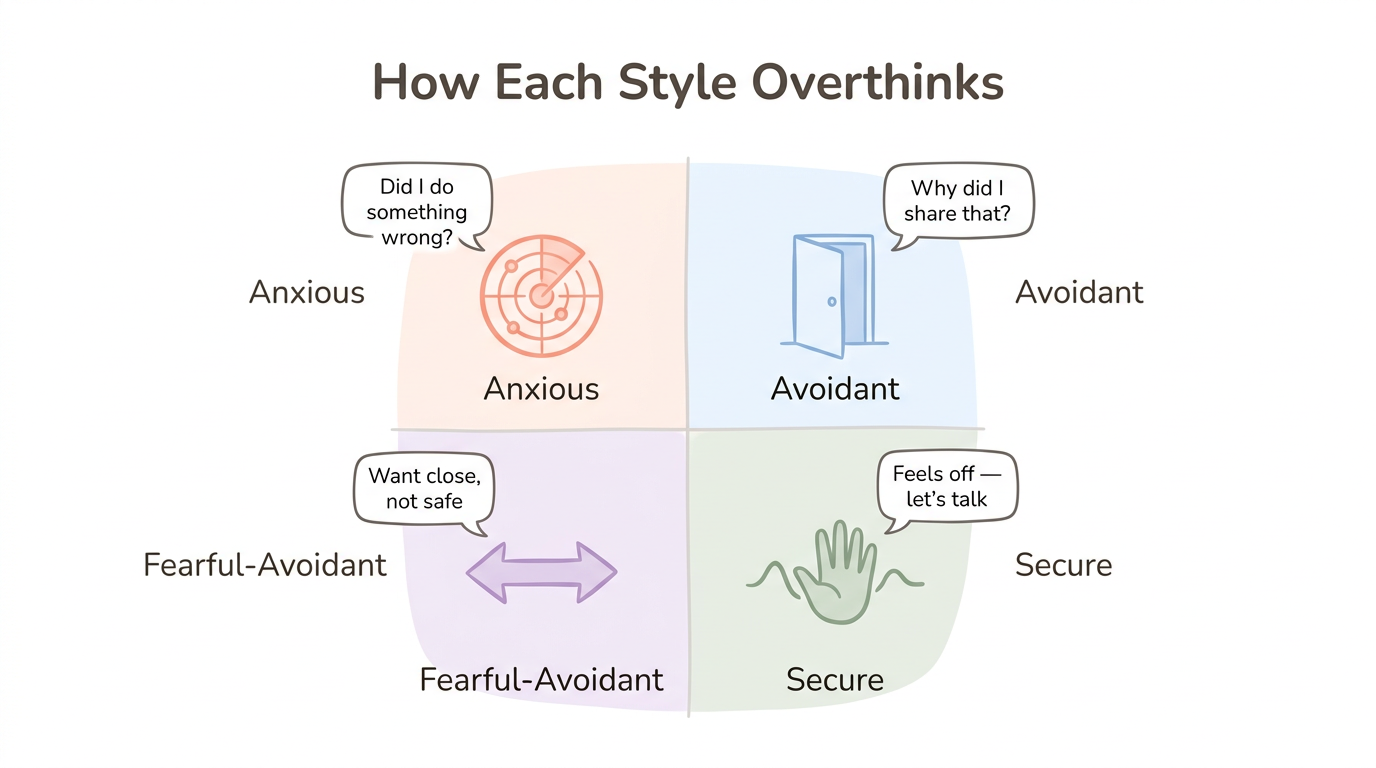
1. Anxious Attachment: The Hypervigilant Scanner
"They're pulling away — what did I do wrong?" That thought, arriving unbidden at 2 a.m. after a perfectly normal evening, is the hallmark of anxious overthinking.
If you have anxious attachment, your hyperactivating strategies keep the attachment system chronically on (Mikulincer and Shaver, 2003). You scan for abandonment cues, replay texts for hidden meaning, and seek reassurance loops. Attachment anxiety is also associated with less mindfulness and more rumination during conflict — in a study of 360 participants, the mindfulness-to-rumination pathway significantly predicted all six conflict outcomes measured (Herring et al., 2020).
2. Avoidant Attachment: The Post-Withdrawal Analyzer
Avoidant overthinking is invisible because it happens privately. After deactivating and then analyzing, you might ruminate on why you pulled away, intellectualize your emotions, or replay vulnerable moments with regret. Attachment avoidance does not directly predict rumination — instead, it reduces mindfulness, which then increases rumination (Herring et al., 2020). The overthinking is real; it just happens behind a calm exterior.
Characteristic thought: "Why did I share that? I shouldn't need them this much."
3. Fearful-Avoidant Attachment: The Oscillator
The oscillating pattern of fearful-avoidant attachment produces the most distressing form of overthinking. You swing between anxious rumination ("they'll leave") and avoidant suppression ("I don't care anyway"), sometimes within the same hour. Emotional intelligence — specifically the ability to perceive and manage emotions — partially mediates this pattern (Lanciano et al., 2012), which explains why these spirals feel so confusing.
Characteristic thought: "I want them close but it's not safe."
4. Secure-Leaning Under Stress: The Temporary Spiral
Even people with earned secure attachment can temporarily overthink during major life transitions or when partnered with someone whose attachment style triggers old patterns. The difference: secure-leaning overthinking resolves into direct conversation rather than escalating into behavioral patterns. The characteristic thought captures this well — "This feels off. Let me think about it — and then talk to them" — reflection that moves toward action rather than spiraling.
| Dimension | Anxious | Avoidant | Fearful-Avoidant | Secure (Under Stress) |
|---|---|---|---|---|
| Core fear | Abandonment / rejection | Loss of autonomy | Both simultaneously | Temporary threat to stability |
| When it peaks | During distance or silence | After intimacy or vulnerability | Unpredictably, both triggers | Major life transitions |
| Behavioral expression | Reassurance-seeking, text monitoring | Withdrawal, intellectualizing | Push-pull cycling, testing | Reflection followed by conversation |
| Nervous system state | Sympathetic activation (fight/flight) | Dorsal vagal (shutdown) | Oscillating between both | Briefly leaves ventral vagal, returns quickly |
| Most effective intervention | Worry Window + self-soothing | Journaling to reconnect with feelings | Pendulation + "Which Voice Is Talking?" | Brief mindfulness check-in |
"Which Voice Is Talking?" Journal Prompt (for all attachment styles)
- Write down a recent overthinking spiral — the specific thoughts that looped
- Label each thought with a letter: (A) Anxious alarm ("They're going to leave"), (V) Avoidant shield ("I shouldn't need them this much"), or (S) Secure observer ("I feel hurt and I can address this")
- Notice which voice dominates your list
- Ask yourself: "What would the Secure observer say about this situation?"
- Write one sentence from the Secure observer's perspective
This builds metacognitive awareness of attachment-driven thought patterns. By labeling each thought, you interrupt automatic identification with the anxious or avoidant voice and strengthen the secure observer — the part of you capable of holding both feeling and perspective simultaneously.
Is It Overthinking or Is Something Actually Wrong?
The distinction between attachment alarm and intuition comes down to one question: is the worry about you or about their behavior? Attachment alarms center on your worthiness ("Am I enough?" "Did I say something wrong?" "Are they losing interest?"). Genuine concerns center on observable actions ("They said they were working late but their location showed somewhere else").
Your overthinking part is not your enemy. Through an Internal Family Systems lens (Schwartz), the inner critic driving your rumination is a protective Manager part — it learned to scan for danger because, at some point in your history, not scanning had consequences. Meeting this part with curiosity rather than frustration is the first step toward changing the pattern.
That said, you need a concrete way to sort stories from evidence in the moment. Here is the framework:
Signals it is an attachment alarm:
- The worry is about your worth, not their actions
- You have felt this same fear in previous relationships
- The intensity does not match the situation
- You feel compelled to seek reassurance immediately
Signals something may genuinely be wrong:
- Your concern is about a specific, observable behavior
- The pattern is new, not a familiar feeling from past relationships
- Other people in your life have noticed the same concern
- You feel clarity rather than panic when you sit with it
"The Evidence Audit" (primarily for anxious attachment)
- Write the worry at the top of a page
- Draw two columns: "Observable Evidence" (things you have directly seen or heard) and "Stories I'm Adding" (interpretations, assumptions, predictions)
- Fill in both columns honestly
- If the left column is sparse, you are likely experiencing an attachment alarm — try a self-soothing technique before acting
- If the left column contains substantial, specific observations, you may need a direct conversation with your partner
This works for anxious attachment because it interrupts the hyperactivating strategy by grounding you in observable reality. Your nervous system is generating urgency based on interpretation — the Evidence Audit forces a slower, prefrontal-cortex-driven assessment instead of an amygdala-driven reaction.
What Are the Most Effective Techniques to Stop Relationship Rumination?
Your nervous system learned to ruminate for a reason — it was trying to solve a problem that felt unsolvable. Honoring that intention while redirecting the strategy is more effective than trying to force your mind to stop.
Rumination-specific techniques outperform general CBT by nearly double — a 2025 transdiagnostic meta-analysis of 55 studies (N = 4,970) found that interventions targeting repetitive negative thinking directly achieved an effect size of g = −0.99 compared to g = −0.56 for general CBT (p = .002). Each additional session increased the effect size by 0.04, meaning consistency matters more than intensity. The techniques below are organized from immediate (use right now) to sustained (build over time).
Scheduled Worry Time: The Metacognitive Approach
Wells' metacognitive therapy research shows that trying to suppress rumination backfires. The principle here is "postpone, don't suppress" — you are not telling your brain the worry does not matter, you are telling it "not right now."
"Worry Window" Scheduling Practice (for anxious attachment)
- Choose a 15-minute daily window — not before bed, ideally mid-afternoon
- When overthinking arises outside this window, write the thought on a designated list and say internally: "I'll get to you at 3 p.m."
- During the window, review the list. Notice how many worries have already lost their charge
- After 15 minutes, close the notebook and do something physical — a walk, stretching, washing dishes
This channels the hyperactivating strategy into a contained space rather than fighting it. Anxious attachment drives a sense of urgency around relational worries — the Worry Window honors that urgency by guaranteeing the worry will be addressed, which paradoxically reduces the need to address it immediately.
Cognitive Defusion: Watching Thoughts Instead of Believing Them
Rather than arguing with your thoughts, observe them as mental events. When the thought "they're losing interest" arises, rephrase it: "I'm having the thought that they're losing interest." This small linguistic shift engages the prefrontal cortex and loosens the thought's grip.
Why Movement Breaks the Loop
Rumination thrives in stillness. Research on self-soothing for anxious attachment consistently shows that physical engagement — not distraction for its own sake, but meaningful activity — breaks the cortisol feedback loop. Even a ten-minute walk changes your neurochemistry enough to shift perspective.
Mindfulness as a Long-Term Rewire
Mindfulness-based cognitive therapy reduces rumination with a standardized mean difference of −0.51, and these effects strengthen at follow-up (SMD = −0.61), suggesting that the skills compound over time (MBCT meta-analysis, 2025). The mechanism is direct: mindfulness interrupts the pathway between attachment anxiety and rumination by increasing present-moment awareness (Herring et al., 2020).
How Can You Calm Your Body to Quiet Your Mind?
Regulate the body first, and thoughts quiet naturally. Rumination is the cognitive expression of a dysregulated nervous system — your mind is trying to think its way to safety because your body feels unsafe. Somatic approaches work by addressing the root activation rather than the mental symptoms.
Through a polyvagal-informed lens, overthinking maps to sympathetic activation — your fight-or-flight system scanning for relational threats. The goal is returning to ventral vagal — the state where your social engagement system comes online and connection feels safe rather than dangerous. (Note: while polyvagal theory's specific neuroanatomical claims face scientific criticism, the clinical framework remains widely used for its practical utility.)
Three body-based techniques can interrupt the rumination-activation cycle:
What does your body do when a text goes unanswered for hours? Maybe your chest tightens, your jaw clenches, your breathing shallows. Vagal toning works directly on that physical response: inhale for 4 counts, exhale for 8 counts. The longer exhale signals safety to your brainstem in a way that cognitive reassurance cannot.
Orienting is deceptively simple. Slowly turn your head and look around the room. Let your eyes rest on objects. This ancient survival mechanism tells your nervous system that you are not in immediate danger — your environment is safe enough to explore visually rather than freeze or flee.
Then there is pendulation, a Somatic Experiencing technique (Levine) especially powerful for fearful-avoidant patterns where the nervous system toggles between hyperactivation and shutdown.
"Pendulation Reset" (for all attachment styles, especially fearful-avoidant)
- Notice where overthinking creates tension in your body — chest tightness, jaw clenching, stomach knots
- Place a hand there. Breathe into that area for 3 to 4 breaths
- Now find a part of your body that feels neutral or calm — your feet on the floor, your hands resting in your lap, the weight of your back against the chair
- Slowly alternate your attention between the tense area and the calm area, spending 3 to 4 breaths on each
- Repeat for 3 full cycles, noticing whether the tension begins to soften
Pendulation teaches your nervous system that activation is not permanent — it can move between states. For fearful-avoidant attachment, where the system gets stuck oscillating between hyperactivation and shutdown, pendulation provides a controlled, gentle version of that oscillation. Over time, the swings become less extreme.
How Does Your Partner's Attachment Style Fuel Your Overthinking?
The most powerful driver of relationship overthinking is often not inside your own head — it is the dynamic between your attachment style and your partner's. The pursue-withdraw cycle is the most well-documented pattern: an anxiously attached partner seeks closeness and reassurance, which triggers an avoidantly attached partner to withdraw, which triggers more anxious pursuit and rumination (Johnson, EFT research).
When your partner goes quiet after a disagreement, your nervous system does not register "they need space." It registers "threat — connection is breaking." Every minute of silence becomes raw material for the rumination machine. If your partner has avoidant attachment, their withdrawal is not personal — it is their own attachment system activating. Understanding this intellectually is one thing. Feeling it in your body is another.
Co-regulation — a partner's calm, present engagement — can activate the ventral vagal pathway and genuinely soothe your nervous system. But here is the critical distinction: co-regulation is not the same as reassurance-seeking. Co-regulation happens when both partners are regulated enough to offer presence. Reassurance-seeking is outsourcing regulation to your partner — asking them to manage your anxiety for you. It works temporarily but reinforces the overthinking cycle long-term, because it teaches your nervous system that you cannot handle distress alone.
Research on oxytocin reveals a paradox relevant here: while oxytocin promotes bonding, it can also intensify negative memory replay and rumination on stressful relational events. This means the very closeness you crave can sometimes amplify the overthinking — especially if the relationship has become the primary site of your emotional regulation.
Learning to communicate needs without triggering your partner means expressing vulnerability as a feeling statement rather than a test or accusation. "I'm feeling disconnected" lands differently than "Why haven't you texted me back?"
"The Pursue-Pause Protocol" (for anxious attachment)
- Notice the urge to seek reassurance — the pull to send a "checking in" text, ask "are we okay?", or test your partner's response
- Pause for 10 minutes. Set a timer if you need to
- During the pause, name what you feel in your body (tight chest, racing heart, stomach dropping)
- Ask yourself: "What am I actually afraid of right now?" Write the answer down
- Try one self-soothing technique — extended exhale breathing, the Pendulation Reset, or placing a hand on your chest
- After 10 minutes, check in with yourself. If the need is still there, express it as a feeling statement: "I'm feeling disconnected and would love to hear from you" rather than "Why aren't you answering me?"
This interrupts the reassurance-seeking loop while honoring the underlying need for connection. Anxious attachment drives a sense that you must act immediately or the relationship will break. The 10-minute pause teaches your nervous system that the relationship can survive a brief delay — and that you can tolerate distress without immediately outsourcing it. Over time, the pause gets easier, and the urgency decreases.
If you recognize the anxious-avoidant trap in your relationship, know that both partners' nervous systems are reacting to each other in a self-reinforcing loop. Breaking it requires both people to understand their own attachment patterns — not just the overthinker making changes alone.
When Should You Seek Professional Help for Relationship Overthinking?
Professional support becomes important when overthinking crosses from occasional discomfort into persistent disruption of your daily life. Research shows that 21 percent of people report being unable to stop ruminating despite wanting to — if that resonates, therapy is not a luxury but a targeted intervention.
Your experience of feeling stuck in these loops makes sense. Your brain built powerful neural pathways around this pattern, and asking yourself to dismantle them alone is like asking yourself to perform surgery on your own arm. A trained therapist provides the relational safety and structured techniques that make change possible.
Seek support if you recognize three or more of these signs:
"The Overthinking Impact Inventory" (for all attachment styles)
Rate each item on a 1 to 5 scale (1 = rarely, 5 = constantly):
- How many hours per day does relationship overthinking consume your attention?
- How often does it disrupt your sleep?
- How often does it lead to conflict with your partner?
- How often do you check your partner's social media or location?
- How much does it affect your work or friendships?
A total score of 15 or higher suggests professional support would be beneficial. A score of 20 or higher suggests it is urgent.
This normalizes help-seeking by making the threshold concrete rather than shame-based. You are not "too broken" for therapy — you have a score on a scale, and that score tells you something useful about what level of support would match your current experience.
Which therapy modality matches your pattern:
- Rumination-Focused CBT (Watkins, 2016): Best for persistent brooding. The effect size nearly doubled compared to standard CBT (g = −0.99 versus g = −0.56 in a 2025 meta-analysis). Specifically targets rumination as a mental habit rather than addressing surface-level thoughts.
- Mindfulness-Based Cognitive Therapy: Sustained effects at follow-up — the SMD actually strengthened from −0.51 during treatment to −0.61 at follow-up (MBCT meta-analysis, 2025). Skills compound over weeks and months.
- Emotionally Focused Therapy (Johnson): Best for couples caught in the pursue-withdraw cycle. Medium effect sizes post-treatment. Addresses the attachment bond directly rather than treating overthinking as an individual problem.
- Somatic therapies: Best for trauma-based overthinking where the body holds activation that cognitive approaches alone cannot reach.
Developing secure attachment as an adult is a gradual process. You do not rewire attachment in a single insight. You rewire it by noticing 10 percent earlier, responding 10 percent differently, 10 percent more often.
Frequently Asked Questions
Is overthinking a sign of anxiety or a relationship problem?
Overthinking can signal both. Attachment-driven overthinking activates regardless of relationship quality — it is your nervous system responding to perceived threat, not actual danger. If overthinking persists across multiple healthy relationships, it likely reflects attachment anxiety rather than a partner-specific issue.
Can overthinking ruin a good relationship?
Yes. Chronic rumination often triggers reassurance-seeking or accusatory behaviors that push partners away, creating the very abandonment the overthinker fears. Research shows rumination mediates the path from attachment insecurity to relationship distress (Burnette et al., 2009). Addressing overthinking directly protects otherwise strong relationships.
What attachment style overthinks the most?
Anxious attachment is most associated with relationship rumination due to hyperactivating strategies that keep the threat-detection system chronically active (Mikulincer and Shaver, 2003). However, avoidant and fearful-avoidant styles also overthink — they do it more privately, often after withdrawing from connection. The difference is not whether overthinking happens but how and when it surfaces.
Is overthinking a trauma response?
Often, yes. Overthinking can be a protective strategy developed in childhood when a caregiver was unpredictable. The brain learned to scan for danger constantly — and that scanning became automatic. Somatic therapies and attachment-focused work address the nervous system roots rather than just the cognitive symptoms.
How do I stop overthinking after an argument?
First, regulate your nervous system — try extended exhale breathing (inhale for 4 counts, exhale for 8 counts) for two minutes. Then use the Evidence Audit: write what actually happened versus the stories you are adding. Wait at least 20 minutes before revisiting the conversation with your partner, giving both nervous systems time to return to baseline.
Why do I overthink more at night?
Cortisol follows a circadian pattern, dropping at night while melatonin rises. This shift reduces your prefrontal cortex's ability to regulate the amygdala's threat signals. Fewer distractions also mean the default mode network runs unchecked. A brief body scan or the Pendulation Reset before bed can interrupt this pattern.
How do I know if I'm overthinking or if something is actually wrong?
Check whether your worry centers on observable behavior ("they lied about their plans") or on interpretation ("they paused before saying 'I love you'"). Attachment alarms focus on your worthiness; genuine concerns focus on specific actions. Use the Evidence Audit exercise to separate observable facts from the stories you are adding.
Can therapy help with relationship overthinking?
Strongly yes. Rumination-focused CBT shows nearly double the effect size of general CBT (g = −0.99 versus g = −0.56). Mindfulness-based cognitive therapy reduces rumination with effects that strengthen over time (SMD = −0.61 at follow-up). For couples caught in the pursue-withdraw cycle, emotionally focused therapy directly addresses the attachment dynamics fueling overthinking.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Attachment Theory and Rumination
-
Mikulincer, M., & Shaver, P. R. (2003). The attachment behavioral system in adulthood: Activation, psychodynamics, and interpersonal processes. Advances in Experimental Social Psychology, 35, 53–152.
-
Burnette, J. L., Davis, D. E., Green, J. D., Worthington, E. L., & Bradfield, E. (2009). Insecure attachment and depressive symptoms: The mediating role of rumination, empathy, and forgiveness. Personality and Individual Differences, 46(3), 276–280.
-
Herring, T., Bhullar, N., & Dunstan, D. A. (2020). Investigating the role of mindfulness and rumination as mediators of the relationship between attachment styles and conflict outcomes. International Journal of Environmental Research and Public Health, 17(19), 7295.
-
Lanciano, T., Curci, A., Kafetsios, K., Elia, L., & Zammuner, V. L. (2012). Attachment and dysfunctional rumination: The mediating role of emotional intelligence abilities. Personality and Individual Differences, 53(6), 753–758.
Neuroscience
-
Hamilton, J. P., Farmer, M., Fogelman, P., & Gotlib, I. H. (2015). Depressive rumination, the default-mode network, and the dark matter of clinical neuroscience. Biological Psychiatry, 78(4), 224–230.
-
Zhou, H. X., Chen, X., Shen, Y. Q., Li, L., Chen, N. X., Zhu, Z. C., ... & Yan, C. G. (2020). Rumination and the default mode network: Meta-analysis of brain imaging studies and implications for depression. NeuroImage, 206, 116287.
-
Kim, M. J., & Whalen, P. J. (2009). The structural integrity of an amygdala–prefrontal pathway predicts trait anxiety. Journal of Neuroscience, 29(37), 11614–11618.
-
Zoccola, P. M., & Dickerson, S. S. (2012). Assessing the relationship between rumination and cortisol: A review. Journal of Psychosomatic Research, 73(1), 1–9.
Treatment Efficacy
-
Transdiagnostic meta-analysis (2025). The effect of cognitive behavioral therapy on repetitive negative thinking: A meta-analysis. PMC, 55 studies, N = 4,970.
-
MBCT meta-analysis (2025). Mindfulness-based cognitive therapy for rumination reduction: A systematic review and meta-analysis. PMC.
-
Watkins, E. R. (2016). Rumination-Focused Cognitive-Behavioral Therapy for Depression. Guilford Press.
-
Johnson, S. M. (2004). The Practice of Emotionally Focused Couple Therapy: Creating Connection (2nd ed.). Brunner-Routledge.
Epidemiology
-
Nolen-Hoeksema, S. (2003). Women Who Think Too Much: How to Break Free of Overthinking and Reclaim Your Life. Henry Holt and Company.
-
Johnson, D. P., & Whisman, M. A. (2013). Gender differences in rumination: A meta-analysis. Personality and Individual Differences, 55(4), 367–374.
-
PMC qualitative survey (2022). Self-reported triggers and coping strategies for repetitive negative thinking. PMC.
Clinical Frameworks
-
Schwartz, R. C. (1995). Internal Family Systems Therapy. Guilford Press.
-
Levine, P. A. (1997). Waking the Tiger: Healing Trauma. North Atlantic Books.
-
Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation. W. W. Norton.
-
Wells, A. (2009). Metacognitive Therapy for Anxiety and Depression. Guilford Press.
This article is for educational purposes only and is not a substitute for professional mental health care. If you are experiencing persistent distress, please consult a licensed therapist or counselor. The techniques described here are informed by research but should be adapted to your individual needs with professional guidance.
