Relationship anxiety is a pattern of persistent fear and insecurity within a romantic bond, rooted in hyperactivation of the attachment system—a learned survival strategy, not a personality flaw (Mikulincer and Shaver, 2003). A 7-year longitudinal study of 2,057 people found that perceived partner gratitude predicted reduced attachment anxiety one year later, independent of relationship satisfaction (Park et al., 2019).
If you love someone who carries this kind of anxiety, you already know the exhaustion of wanting to help but feeling like nothing you do is quite enough. This article is not a list of surface-level tips. It is evidence-based guidance that treats both partners' needs—yours and theirs—by helping you understand the underlying dynamics that make everything else click. Whether your partner's anxiety feels new or long-standing, the research points to specific, actionable ways you can shift the pattern together.
Key takeaway: Relationship anxiety reflects attachment system hyperactivation, not a character flaw. The most effective partner support combines responsive validation without excessive accommodation, co-regulation through your own calm nervous system, and specific expressed gratitude that counters the core fear of being unworthy. A single psychoeducational session about these dynamics reduces both reassurance-seeking and partner accommodation.
What is relationship anxiety and why does your partner experience it?
Relationship anxiety is hyperactivation of the attachment system—an amplification of distress signals developed to maintain closeness with caregivers who were inconsistently available. Your partner's brain learned early that love was unpredictable, so it developed a vigilance system that scans for threats to the bond (Mikulincer and Shaver, 2016). This is not a character flaw. It is a learned survival strategy that once served a real purpose.
What makes relationship anxiety different from generalized anxiety is its specificity. Your partner may function calmly in most areas of life but become flooded when they perceive—even unconsciously—a threat to your connection. A delayed text, a shift in your tone, a cancelled plan. Neuroimaging research shows that anxiously attached individuals display increased amygdala activation and heightened affective evaluation compared to securely attached individuals, meaning their emotional processing system is tuned to a higher sensitivity for relationship threat signals.
Understanding what triggers your partner's anxiety is the first step toward responding effectively rather than reactively. Their nervous system is not choosing to overreact. It is doing exactly what it was trained to do.
The Origin Story Conversation (for both partners)
- Set aside 20 minutes in a calm, private space
- The partner with anxiety shares one early memory where closeness felt unreliable or unsafe
- The supporting partner listens without fixing, advising, or explaining
- Reflect back what you heard: "It sounds like you learned that..."
- The anxious partner says what it was like to be heard this way
Being fully heard without judgment directly counters the early experience of having needs dismissed or met inconsistently—that is the corrective emotional experience anxious attachment needs most. If your partner recognizes these patterns, they might also explore the 12 signs of anxious attachment.
Why does reassurance help in the moment but not long-term?
Excessive reassurance does not actually reduce attachment insecurity—it reinforces the belief that reassurance is constantly needed. Shaver, Schachner, and Mikulincer (2005) tracked 61 couples over 14 days using daily diaries and found that excessive reassurance seeking did not decrease insecurity in anxiously attached partners. Instead, it maintained their fears and increased relationship conflict.
Your instinct to protect your partner from distress makes sense—that is love in action. The difficulty is that researchers have found this pattern, sometimes called the accommodation trap, can inadvertently work against the very person you are trying to help. When you avoid certain topics, constantly check in before being asked, change plans to prevent triggers, or provide the same verbal reassurance every day, you reduce your partner's anxiety in the short term. But you also communicate an unspoken message: you cannot handle this on your own. Each accommodation prevents the corrective experience your partner needs—the experience of tolerating uncertainty and discovering that the relationship survives it.
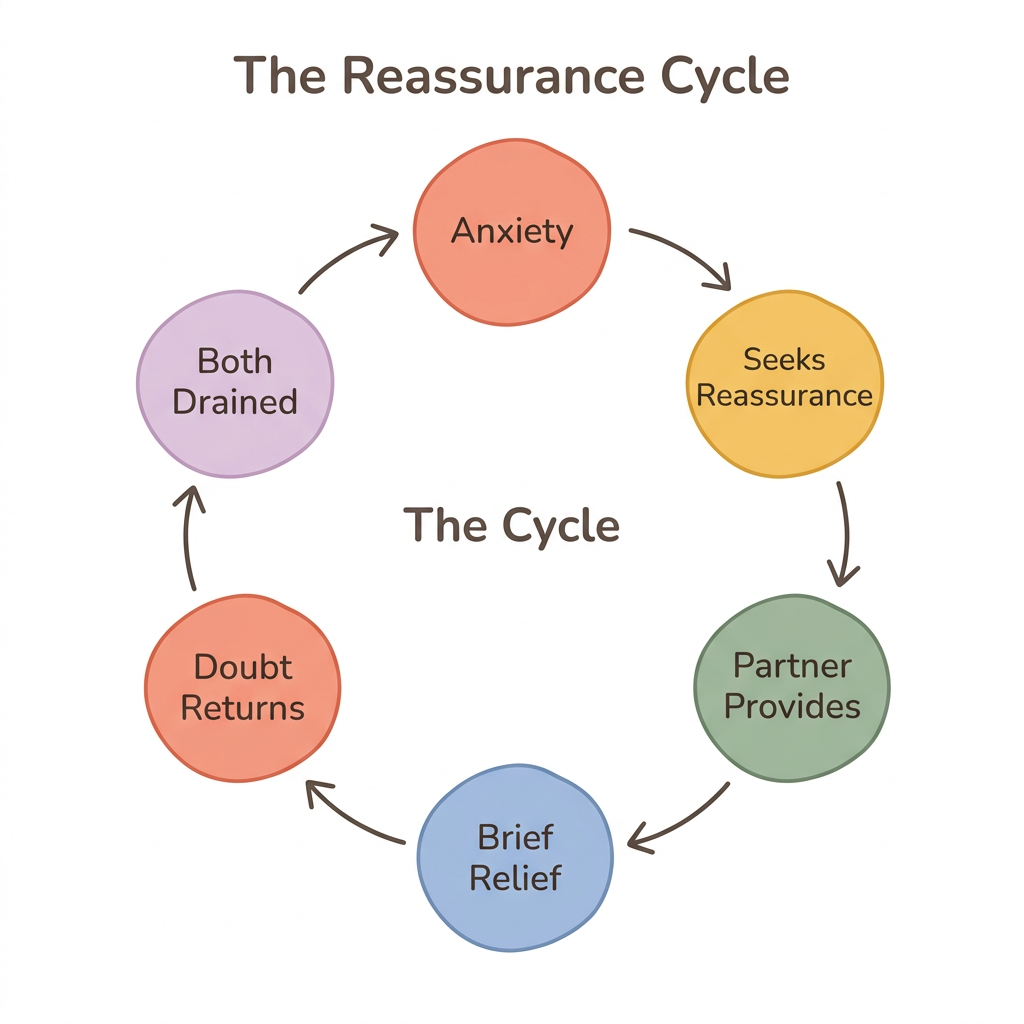
The cycle works like this: anxiety rises, your partner seeks reassurance, you provide it, they feel temporary relief, doubt returns, they seek more, you feel drained, and both nervous systems end up more activated than where they started. Over time, this pattern can strain even a good relationship.
5 signs you may be accommodating your partner's anxiety:
- You avoid mentioning certain friends, coworkers, or social plans to prevent a reaction
- Those unprompted "thinking of you" texts throughout the day are not coming from genuine warmth—they are driven by fear of what happens if you don't send them
- You have changed your routine—cancelled plans, left events early—to manage their worry
- The same question—"Are we okay?"—gets the same answer multiple times a day, and neither of you feels settled by it
- Normal, harmless interactions get hidden because explaining them feels exhausting
The Reassurance Audit (for the supporting partner)
- Write down three things you do regularly to prevent your partner's anxiety
- For each one, ask yourself honestly: does this help them build confidence, or does it communicate "you can't handle this"?
- Circle any that you suspect are accommodation rather than genuine care
- Pick one to discuss with your partner during a calm moment
Building your awareness of the accommodation pattern is the necessary first step before attempting behavior change. The goal is not to withdraw support—it is to recognize where your support may be inadvertently maintaining the cycle.
How can you support your partner without enabling the anxiety cycle?
Responsive validation—attending to your partner's emotional experience without reinforcing catastrophic interpretations—is the evidence-based middle path between dismissing their feelings and accommodating the anxiety. Reis, Clark, and Holmes (2004) defined perceived partner responsiveness as the process by which someone comes to believe their partner attends to and reacts supportively to core features of their self. When your partner perceives you as responsive, their attachment security increases.
Here is what makes this finding powerful: Paprocki and Kashdan (2017) found that a single psychoeducational session—one conversation where both partners learned about the anxiety-reassurance cycle—significantly decreased reassurance-seeking in the anxious partner AND decreased maladaptive accommodation in their partner. Twenty-one couples. One session. Psychoeducation is itself therapeutic. Reading this article together is a version of that intervention.
The practical principle is this: validate the emotion, not the catastrophe. When your partner says "I feel like you're going to leave me," the emotion (fear) is real and deserves acknowledgment. The interpretation (you are leaving) does not need to be reinforced with elaborate evidence to the contrary.
4-Step Response Framework:
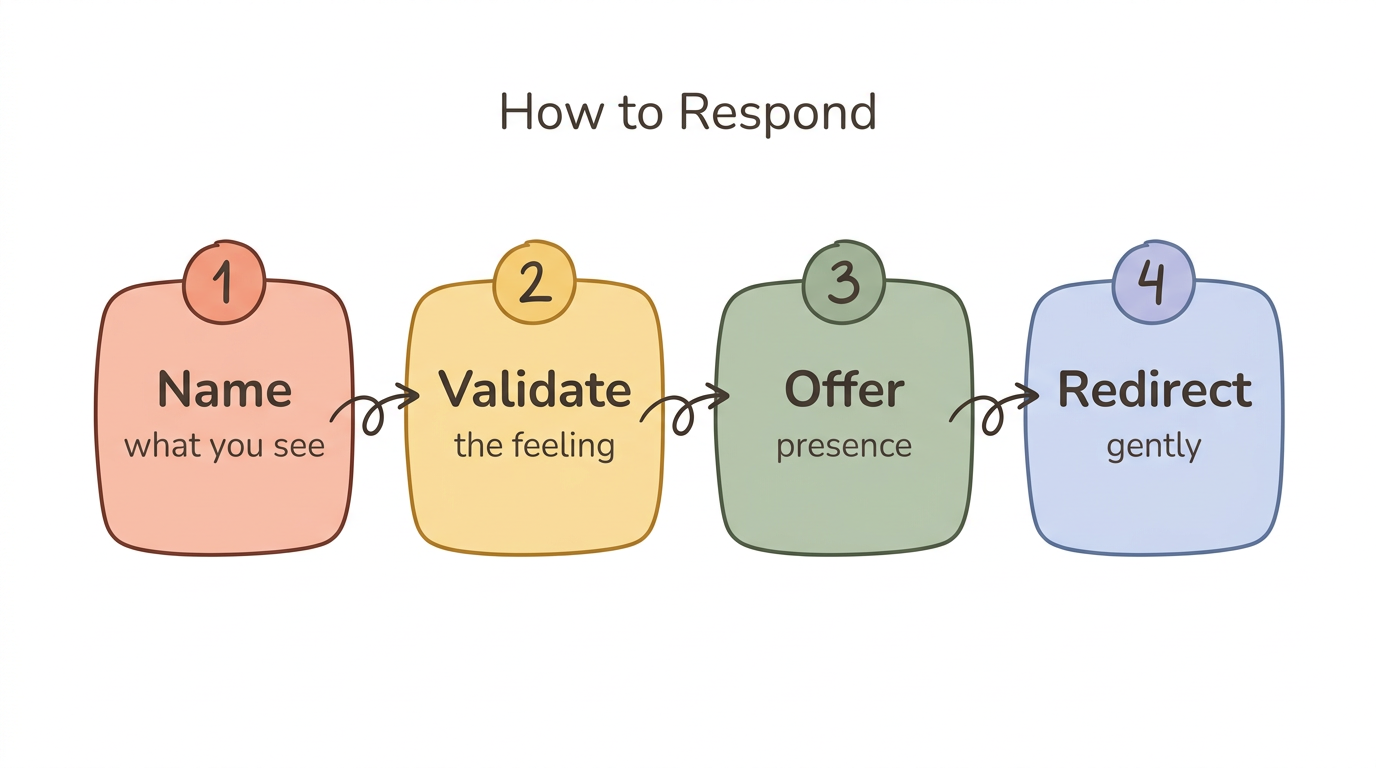
- Name what you see — "I notice you seem worried right now"
- Validate the feeling — "That makes sense given what you've been through"
- Offer presence, not promises — "I'm here. What would feel helpful right now?"
- Redirect gently — "Let's try our grounding exercise together"
For deeper guidance on the communication side, see how to communicate your needs without triggering your partner.
"Ask, Don't Assume" Practice (for the supporting partner — targets anxious attachment)
- Next time your partner seems activated, pause before jumping to reassurance
- Ask: "Would it help if I sit with you right now, or do you need a moment alone?"
- Accept their answer without taking it personally
- Practice this three times this week and note how they respond each time
Hyperactivation often includes a loss of agency—the anxiety feels like it is happening to them. Being asked what they need interrupts that helplessness and gives the anxious partner a sense of choice, which is itself regulating.
What does your partner's nervous system actually need from you?
Your partner's nervous system needs safety cues from your body before it can process safety from your words. Coan and colleagues (2006) conducted fMRI scans on married women while they anticipated electric shock. Holding their husband's hand produced pervasive attenuation of neural threat responses in the prefrontal cortex, anterior cingulate, and caudate. A stranger's hand helped a little. Their partner's hand helped significantly. And here is the key finding: higher relationship quality meant greater neural calming—particularly in the right anterior insula, superior frontal gyrus, and hypothalamus. This was replicated with 110 diverse participants.
The neurochemistry confirms this. Partner touch produces higher oxytocin and lower cortisol compared to stranger touch, with the medial prefrontal cortex acting as a neural hub for stress modulation through social contact.
Porges (2022) explains the mechanism through polyvagal theory: your partner's nervous system detects safety cues—soft vocal prosody, warm facial expressions, calm body language, and physical touch—through a process called neuroception. This is unconscious. Your partner does not decide to feel safer when you speak softly. Their ventral vagal system picks up the signal and shifts from threat to social engagement without conscious thought. Your calm is contagious—not as a metaphor, but as a neurobiological reality.
To understand more about how attachment patterns live in the body, explore how attachment style affects your nervous system.
The 60-Second Co-Regulation Reset (somatic technique — for anxious attachment hyperactivation)
- Regulate yourself first — Take 3 slow exhales, drop your shoulders away from your ears, unclench your jaw
- Move closer with open body language (uncrossed arms, facing them)
- Offer physical contact — a hand on their back, holding their hand, or sitting with your legs touching
- Speak slowly in a lower register — your vocal tone signals safety to their nervous system before your words do
- Match their breathing pace, then gradually slow yours — their system will begin to entrain to your rhythm
Your partner's nervous system detects your regulated state through neuroception and uses it as a template to downshift from sympathetic activation. You cannot co-regulate from a dysregulated state, which is why step one matters most.
How does expressing gratitude reduce your partner's anxiety?
Specific, behavioral gratitude directly counters the core anxious fear—"I am not enough." Park and colleagues (2019) conducted a 7-year longitudinal study of 2,057 people and found that perceiving higher-than-typical gratitude from a partner predicted reduced attachment anxiety one year later. This effect held independent of global relationship satisfaction. The reverse was not true—reduced anxiety did not predict more perceived gratitude. The direction is clear: gratitude signals "you are valued," and that signal reshapes attachment security over time.
The mechanism works because anxious attachment is organized around a fundamental question: Am I worthy of consistent love? Every unanswered text, every distracted evening, every forgotten detail gets filtered through that question. Specific behavioral gratitude provides repeated, concrete evidence that answers it.
What makes gratitude therapeutic is specificity. Generic praise like "thanks for being great" is warm but hard for the anxious mind to hold onto because it is vague—the nervous system needs specifics it can anchor to. "I noticed you made time for dinner with my family even though you were exhausted—that meant a lot because it showed me you care about my world" works because it references a specific behavior your partner chose, which they can repeat and build identity around.
The Specific Gratitude Practice (targets anxious attachment — 1 week)
- Each evening, tell your partner one specific thing they did that day that you appreciated
- Name the behavior (what they did), not a trait (who they are)
- Explain why it mattered to you — connect it to your experience
- Example: "I appreciated that you texted me about your day—it makes me feel included in your life" rather than "thanks for being thoughtful"
- Continue for seven consecutive days and notice any shifts
Each gratitude expression is a data point the anxious nervous system can store as evidence against the "I'm not enough" belief. Unlike reassurance, gratitude is proactive—it arrives before the anxiety does, which makes it easier for the nervous system to receive.
What should you avoid saying or doing?
Well-meaning responses often backfire because they collide with the specific fears that drive anxious attachment. Your intention does not matter to your partner's nervous system—the impact does. Here are five common mistakes and the attachment science behind why each one deepens the wound instead of healing it.
5 things to avoid and why they backfire:
-
"You're overthinking it." Their nervous system hears: your experience is wrong, and you are a burden for having it. Minimizing their emotional reality confirms the anxious core belief that they are "too much."
-
"I've never given you a reason not to trust me." Anxiety is not a rational process that responds to evidence—logic does not override it. Your partner hears an implication that they should be able to think their way out of a nervous system response, which leaves them feeling broken on top of anxious.
-
"If you don't stop this, I'm leaving." The anxious system is scanning for exactly this signal. Ultimatums confirm the deepest abandonment fear and escalate hyperactivation rather than calming it.
-
Withdrawing in frustration. Going silent, leaving the room, emotionally shutting down—withdrawal confirms the anxious belief that their needs push people away. Even if you need space (which is valid), how you take it matters enormously.
-
Providing reassurance on demand, every time. Well-meaning accommodation prevents your partner from developing distress tolerance. It communicates care in the short term and dependency in the long term (Shaver, Schachner, and Mikulincer, 2005).
If you recognize a pursue-withdraw dynamic in your relationship, these patterns may be particularly entrenched.
The Repair Script (for the supporting partner)
- Think of a recent moment you responded unhelpfully to your partner's anxiety
- Write a 2-sentence repair: (a) what you wish you had said instead, and (b) what you would like to try next time
- Share it with your partner when you are both calm
- Example: "When you asked if we were okay last Tuesday and I snapped, I wish I'd said 'I can see you're worried—I'm not going anywhere.' Next time, I want to pause before I react."
Repair is one of the most powerful attachment interventions because it demonstrates that ruptures do not end the relationship—they can strengthen it. Modeling vulnerability this way also gives the supporting partner practice with the emotional risk their anxious partner lives with daily.
How do you take care of yourself while supporting an anxious partner?
Your needs are not secondary to your partner's anxiety. Compassion fatigue is real, and ignoring it does not make you a better partner—it makes a depleted one. When your partner's nervous system is chronically activated, your nervous system is affected too. Emotional contagion means that their dysregulation can pull you into a threat state, and you cannot co-regulate from a dysregulated state.
Your own wellbeing is not a luxury. It is the foundation that makes everything else in this article possible. That might mean your own therapy, friendships that replenish you, exercise, or simply time alone that you do not feel guilty about taking.
Boundaries are for the relationship, not against your partner. Framing matters. "I can reassure you once, and then let's use our grounding exercise together" is different from "I'm not doing this anymore." The first creates a predictable, boundaried structure. The second triggers abandonment. Your partner's nervous system can learn to trust a consistent boundary faster than it can learn to trust unlimited accommodation—because the boundary is the same every time.
Your partner can also build their own skills alongside the work you do together. Self-soothing techniques for anxious attachment and strategies for overthinking give them tools that do not depend on your availability.
The Boundary Blueprint (for both partners)
- One thing you are willing to always do: for example, "I will always tell you where I'm going and when I'll be back"
- One thing you need to stop doing: for example, "I will stop answering the same reassurance question more than once in a conversation"
- One replacement behavior: for example, "After one reassurance, I'll suggest we do our breathing exercise together"
- Write these down and share them during a calm moment—not during a conflict
- Revisit and adjust monthly as you both learn what works
Predictability is regulating; inconsistency—even well-intentioned inconsistency—is activating. By creating boundaried support together, both partners give the anxious nervous system a reliable structure it can learn to trust over time.
When should you seek professional help together?
Self-help reaches its limit when negative cycles have become entrenched, when one or both partners feel burned out, or when the anxiety is worsening despite consistent effort. If you recognize a pursue-withdraw pattern that neither of you can interrupt on your own, that is not failure—it is information that you need a trained third person in the room.
Emotionally focused therapy (EFT) is the gold standard for attachment-based couples work. The research is compelling: 70 to 75 percent of couples fully recover through EFT, and approximately 90 percent experience significant improvements (ICEEFT). A comprehensive meta-analysis found 82 percent stability of change at two-year follow-up, with an effect size of d=1.3—larger than any other couple intervention (Johnson et al., 1999). Research by Beasley and Ager specifically found that couples with higher attachment anxiety benefit more from EFT, not less.
For the individual partner experiencing anxiety, CBT-based approaches can reduce attachment anxiety in approximately 10 weeks. Some couples benefit from both individual and couples therapy running in parallel.
Seeking help is a relationship investment, not evidence that something is broken. The couples who do best in therapy are often the ones who arrive before the relationship is in crisis—when there is still enough goodwill to build on. You can explore more about whether an anxious-avoidant dynamic can become secure or learn about therapy options for couples caught in the pursue-withdraw cycle.
The Couples Therapy Readiness Check (for both partners)
- Together, answer honestly: Have our negative cycles gotten worse in the last 3 months?
- Do we both feel heard when we try to discuss the anxiety?
- Has our self-help work helped, or have we plateaued?
- If answers suggest stuckness, agree on one concrete next step—research EFT therapists in your area, book a consultation call, or ask your individual therapist for a referral
Making this decision collaboratively matters. When the anxious partner is the one pushing for therapy, it can feel like another form of reassurance-seeking. When both partners decide together, it becomes a shared investment in the relationship rather than one person's project.
Helpful vs. harmful partner responses to relationship anxiety
| Situation | Harmful Response (and Why) | Helpful Response (and Why) |
|---|---|---|
| Partner asks "Do you still love me?" for the third time today | Snapping "I already told you!" (confirms they are a burden) | "I love you. I notice this worry keeps coming back—what would help you feel settled right now?" (validates and redirects) |
| Partner gets upset you did not text back quickly | "I was in a meeting, relax" (minimizes and dismisses) | "I can see the wait was hard. I'm here now." (names their experience and offers presence) |
| Partner wants to check your phone | Handing it over every time (accommodation trap) | "I understand the worry. I won't hide anything, but checking won't solve what's underneath this. Can we talk about what triggered it?" (validates and avoids accommodation) |
| Partner spirals before you go out with friends | Cancelling your plans (reinforces the belief that their needs push you away long-term) | "I'm going and I'll check in at 9pm. I want you to have a good evening too—what's your self-care plan?" (predictable boundary and agency) |
| Partner interprets your quietness as anger | "I'm just tired, not everything is about you" (shame-inducing) | "I'm in a quiet mood tonight—it's not about us. Want to just sit together?" (names internal state and offers connection) |
Frequently Asked Questions
How do I reassure my partner without enabling their anxiety?
Validate their emotion once with warmth—"I hear you, that feeling is real"—then redirect to a coping strategy rather than repeating reassurance. Research shows one meaningful validation outperforms repeated verbal reassurance, which maintains anxiety long-term by preventing your partner from building distress tolerance (Shaver, Schachner, and Mikulincer, 2005).
Can you love someone and still have relationship anxiety?
Yes. Relationship anxiety reflects attachment system activation, not the absence of love. Anxiously attached individuals often experience more intense love alongside more intense fear. The anxiety signals how much the relationship matters to them, filtered through earlier experiences of inconsistent caregiving (Mikulincer and Shaver, 2016).
What does relationship anxiety feel like to the other partner?
Partners often describe feeling constantly tested, walking on eggshells, or never able to provide enough reassurance. Over time this creates compassion fatigue and emotional exhaustion. Both partners' nervous systems become affected through emotional contagion (Simpson and Overall, 2014), making co-dysregulation a shared experience rather than one person's problem.
Should I tell my partner about my relationship anxiety?
Yes, and framing matters. Share it as information about your nervous system, not a demand for behavior change. Try: "Sometimes my brain tells me you're pulling away even when you're not—that's my anxiety, not reality. Here's what helps me." Research shows psychoeducation alone reduces both reassurance-seeking and accommodation (Paprocki and Kashdan, 2017).
How do I set boundaries with an anxious partner without making them feel abandoned?
Frame boundaries as for the relationship, not against your partner. State what you will do, not just what you will not: "I can reassure you once, and then let's try our breathing exercise together." Consistent, predictable boundaries reduce anxiety over time because they create a reliable pattern your partner's nervous system can trust.
Is relationship anxiety a mental illness?
Relationship anxiety is not a formal diagnosis in the DSM-5. It is a pattern of attachment-related distress that exists on a spectrum. When it becomes persistent and significantly impairing, it may overlap with generalized anxiety disorder or relationship OCD. Regardless of diagnostic category, it responds well to therapy—particularly emotionally focused therapy and CBT.
Can couples therapy help relationship anxiety?
Yes, and it may be the most effective option. Emotionally focused therapy has a 70 to 75 percent full recovery rate for distressed couples, with 82 percent stability at two-year follow-up (ICEEFT; APA PsycNet, 2023). Research specifically shows that couples where one partner has higher attachment anxiety benefit more from EFT, not less (Beasley and Ager).
What not to say to someone with relationship anxiety?
Avoid "you're overthinking it" (dismisses their reality), "I've never given you a reason not to trust me" (treats anxiety as rational when it is not), and "if you don't stop, I'll leave" (directly activates the abandonment fear). Validate the emotion while gently challenging the interpretation—"I can see you're worried. What would help right now?"
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Attachment Theory and Core Research
-
Mikulincer, M., & Shaver, P. R. (2003). Attachment in adulthood: Structure, dynamics, and change. Guilford Press.
-
Mikulincer, M., & Shaver, P. R. (2016). Attachment in adulthood: Structure, dynamics, and change (2nd ed.). Guilford Press.
-
Mikulincer, M., & Shaver, P. R. (2020). Broaden-and-build effects of contextually boosting the sense of attachment security in adulthood. Current Directions in Psychological Science, 29(1), 22–26.
-
Reis, H. T., Clark, M. S., & Holmes, J. G. (2004). Perceived partner responsiveness as an organizing construct in the study of intimacy and closeness. In D. J. Mashek & A. Aron (Eds.), Handbook of closeness and intimacy. Lawrence Erlbaum Associates.
Reassurance-Seeking and Accommodation
-
Shaver, P. R., Schachner, D. A., & Mikulincer, M. (2005). Attachment style, excessive reassurance seeking, relationship processes, and depression. Personality and Social Psychology Bulletin, 31(3), 343–359.
-
Accommodating anxiety in romantic relationships. (2024). Psychology Today.
Interventions and Therapy Research
-
Paprocki, C. M., & Kashdan, T. B. (2017). A single psychoeducational session for partners reduces reassurance seeking and accommodation. Family Process, 56(4), 866–881.
-
Park, Y., Johnson, M. D., MacDonald, G., & Impett, E. A. (2019). Perceiving gratitude from a romantic partner predicts decreases in attachment anxiety. Psychological Science, 30(12), 1798–1810.
-
Johnson, S. M., Hunsley, J., Greenberg, L., & Schindler, D. (1999). Emotionally focused couples therapy: Status and challenges. Clinical Psychology: Science and Practice, 6(1), 67–79.
-
ICEEFT. EFT research. International Centre for Excellence in Emotionally Focused Therapy.
-
Beasley, C. C., & Ager, R. Emotionally focused couples therapy: A systematic review of its effectiveness and the role of attachment anxiety. APA PsycNet.
Neuroscience and Somatic Research
-
Coan, J. A., Schaefer, H. S., & Davidson, R. J. (2006). Lending a hand: Social regulation of the neural response to threat. Psychological Science, 17(12), 1032–1039.
-
Partner touch, oxytocin, and cortisol modulation. (2023). PMC.
-
Porges, S. W. (2022). Polyvagal theory: A science of safety. Frontiers in Integrative Neuroscience, 16, 871227.
-
Neuroimaging studies on attachment anxiety and affective evaluation. PMC.
Partner Buffering
- Simpson, J. A., & Overall, N. C. (2014). Partner buffering of attachment insecurity. Current Directions in Psychological Science, 23(1), 54–59. PMC.
This article is for educational purposes only and is not a substitute for professional mental health advice. If you or your partner are experiencing significant distress, please consult a licensed therapist who specializes in attachment-based approaches.
